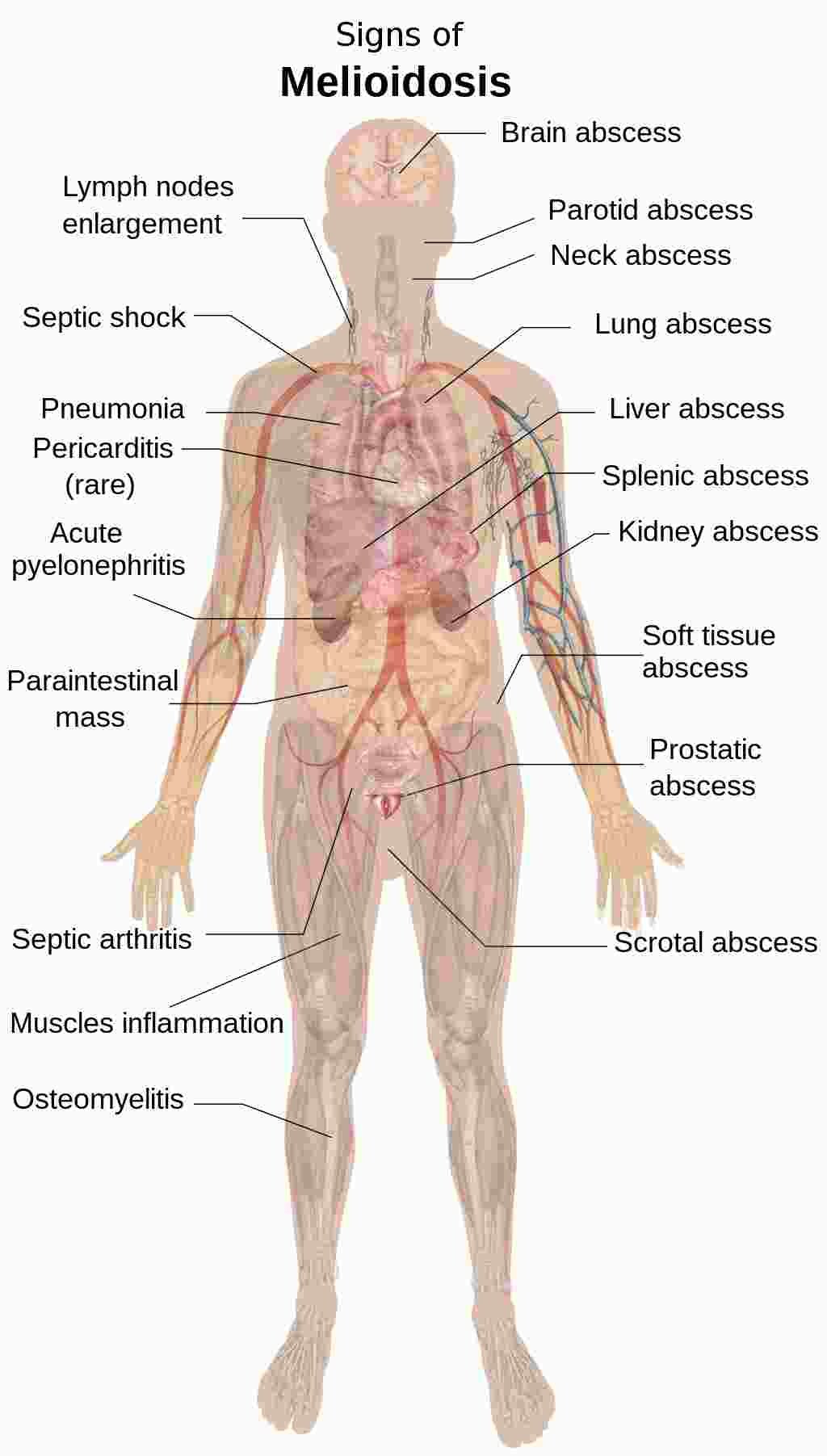
Melioidosis causes pneumonia, abscess formation, or infection
Melioidosis is an infection caused by the gram-negative bacterium Burkholderia pseudomallei (formerly called Pseudomonas). Melioidosis infection may causes pneumonia, sepsis or local infection in various organs. Diagnosis is based on staining and culture. Treatment with antibiotics such as ceftazidime should be prolonged and with a doctor’s prescription.
The risk of contracting melioidosis is highest among adventure travellers, ecotourists, military personnel, construction workers, miners, and others whose contact with contaminated soil or water may expose to bacteria in an endemic area.
Burkholderia pseudomallei can be isolated from soil and water and is endemic to Southeast Asia; Australia; Central, West and East Africa; India; Middle East and China.
Humans can contract melioidosis through contamination on scrapes or burns, by ingestion or inhalation, but not directly from infected animals or people.
In endemic areas, melioidosis can occur when:
- Diabetes
- Alcohol abuse disorder
- Chronic kidney disease
- Immunosuppression including AIDS
Melioidosis is considered a possible agent of bioterrorism.
Key points of Melioidosis
- Melioidosis is contracted through skin contact, ingestion, or inhalation; it is not contracted directly from infected animals or subjects.
- The most common manifestation is an acute (sometimes severe) lung infection, but purulent lesions may occur in the skin and/or many other organs; sepsis, which has a high mortality, may also occur.
- Diagnose by staining and culture; blood cultures are taken but are often negative, except in cases of severe sepsis.
- Treat symptomatic patients with IV ceftazidime followed by an extended course of TMP (trimethoprim)/SMX (sulfamethoxazole) or doxycycline; in children < 8 years and pregnant women, use amoxicillin/clavulanic acid instead of doxycycline.
Read also: Types of Antibiotics and List of Antibiotics

One of the melioidosis abscesses on the abdomen. Isuru Chamika Indeewara Kahandawaarachchi, Gayani Samadara Premawansa, Wipula Warnasuriya, Malka Dassanayake and Enoka Corea, CC BY 4.0, via Wikimedia Commons
Avoid muddy water
Despite everything, the CDC considers that the risk to the general population remains “very low”. They are currently investigating to determine how widespread the bacteria are in the environment.
Symptoms of melioidosis can be broad, such as fever, joint pain, or headache. This can lead to pneumonia, abscess formation, or infection. Worldwide, melioidosis is fatal in 10-50% of cases.
Epidemiology
The disease is endemic in Southeast Asia and northern Australia, but cases are seen particularly in the tropics. In Europe, an increasing number of cases are being reported.
Men are more often affected than women (sex ratio 1.4:1).
Clinical description (signs and symptoms)
Melioidosis can appear at any age, but it is most common between the ages of 40 and 60. The incubation period varies from two days to several months or years.
The acute form of the disease is manifested by respiratory infections (necrotizing pneumonia) and sepsis (with high fever, headache, diarrhea, vomiting, skin lesions and abscesses).
The subacute and chronic forms are characterized by abscesses and suppurative lesions affecting: lungs (simulating tuberculosis), liver, intestine, spleen, but also skin, lymph nodes, brain and bones.
| Presentation Types | Characteristics | |
| Acute | Localized | Acute, local infection (with ulceration) of subcutaneous tissue, lymph nodes, and occasionally salivary glands |
| Pulmonary |
|
|
| Septicemic |
|
|
| Chronic | Asymptomatic |
|
Etiology / analysis
Melioidosis is caused by Burkholderia pseudomallei, a natural saprophyte of moist soils, mud, ponds and rice fields.
Contamination occurs through abrasions, wounds or soiled burns, but also through ingestion or inhalation. Diabetes, kidney failure, thalassemia or high alcohol consumption are often independent risk factors.
Diagnostic method(s)
Diagnosis is based on demonstration of the pathogen identified after culture. Other methods include: haemagglutination, direct immunofluorescence, ELISA, complement fixation or PCR tests.
These methods can also make it possible to estimate the prevalence of infection in a given population. Imaging helps to assess the extent of the disease.
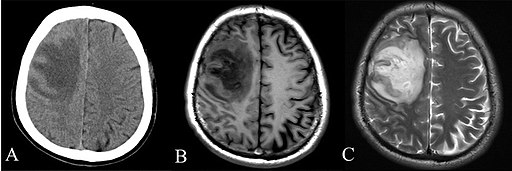
CT and MRI scan of the brain with melioidosis:
– A: CT scan of the brain showing hypodensity of the left frontal lobe of the brain.
– B: T1-weighted MRI scan of the same brain showing hypointensity of the lesion.
– C: T2-weighted MRI scan of the same brain showing hyperintensity of the lesion.
Wei-yuan Huang, Gang Wu, Feng Chen, Meng-meng Li and Jian-jun Li, CC BY 4.0, via Wikimedia Commons
Differential Diagnosis(ies)
The differential diagnoses are tuberculosis, pneumonia and other infectious diseases, such as plague, syphilis and typhoid fever.
Care and treatment
The pathogen is sensitive to a whole series of antibiotics. Treatment consists of an intensive phase of at least two weeks of administration of ceftazidime or meropenem (possibly imipenem) intravenously, followed by a few months of administration of antibiotics by mouth, for example, cotrimoxazole.
Prognosis
The reported mortality rate varies between 15 and 40% of cases, depending in particular on the resources available to treat patients in the different regions of the world. Early diagnosis and adequate treatment are essential. Relapses are possible.

Melioidosis with septic arthritis and left hip joint destruction. N. P. Weerasinghe, H. M. M. Herath and T. M. U. Liyanage, CC BY 4.0, via Wikimedia Commons
Prevention
As the disease is poorly understood, there is little possible prevention, other than limiting exposure. When traveling to one of the endemic areas, it is advisable to protect the skin well in humid areas, especially if it has wounds.
B. pseudomallei seems to be very weakly immunizing and vaccine trials with B. thailandensis, or attenuated strains of B. pseudomallei, have been unsuccessful. The development of a vaccine therefore seems remote and of little interest to the pharmaceutical industries, because the disease remains endemic in poor countries, and it presents a high pathogenic complexity.
Take precautions to protect yourself by:
- Avoid contact with soil or muddy water.
- Wear waterproof boots when gardening.
- Wear gloves to protect the hands when working directly with soil.
Sources: PinterPandai, CDC, National Library of Medicine, Egton Medical Information Systems, CNN, The American Journal of Managed Care (AJMC)
Photo credit: Cerevisae (CC BY-SA 4.0) via Wikimedia Commons