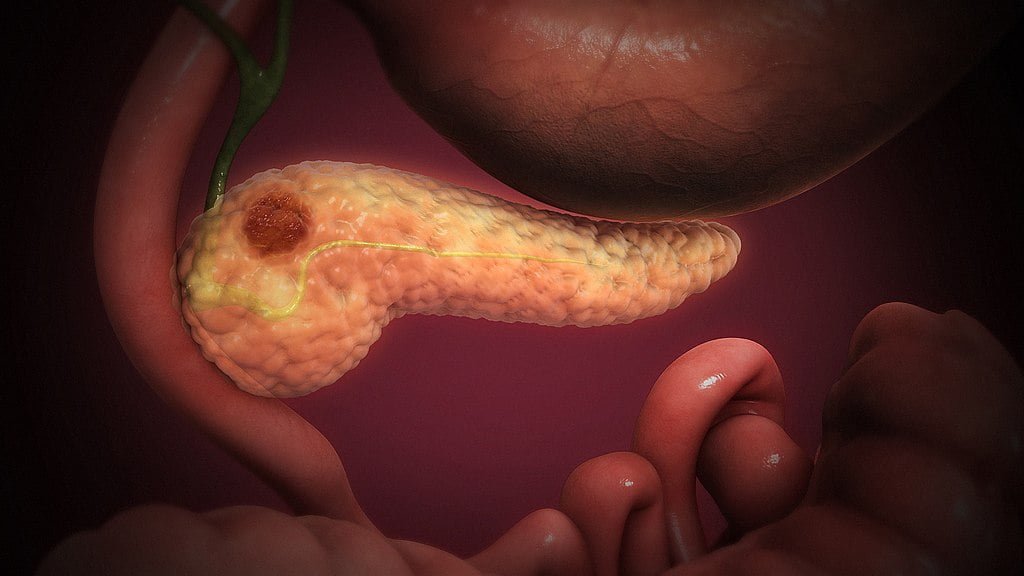
What is pancreatic cancer?
Pancreatic cancer starts in the cells of the pancreas. Cancerous (malignant) tumor is a group of cancer cells that can invade and destroy nearby tissue. It can also spread (metastasize) to other parts of the body.
The cells of the pancreas sometimes undergo changes that make the way they grow or behave abnormally. These changes can lead to the formation of non-cancerous (benign) tumors, such as pancreatic pseudocyst and serous cystic tumor (SCT).
Changes in the cells of the pancreas can also cause precancerous conditions. This means that the abnormal cells are not yet cancerous, but they are likely to become cancer if left untreated. The most common precancerous conditions of the pancreas are mucinous cystic tumor (MCT), mucinous papillary intracanal tumor (MPIT) as well as solid and pseudopapillary tumor.
But in some cases, changes in the cells of the pancreas can cause cancer. Most of the time, pancreatic cancer starts in the cells of the pancreatic duct. This type of cancer is called ductal adenocarcinoma of the pancreas. About 95% of all pancreatic cancers are ductal adenocarcinomas.
There are also rare types of pancreatic cancer such as adenosquamous carcinoma.
Another rare type of tumor can start in the endocrine cells of the pancreas. It is a neuroendocrine tumor of the pancreas (NTp). These tumors are classified as a precancerous tumor or cancerous tumor, called neuroendocrine carcinoma of the pancreas, based on how these cells differ from normal cells (differentiation) and how quickly they grow (grade).
The pancreas is a flat, pear-shaped gland located behind the stomach. It is part of the digestive system. The pancreas is also part of the endocrine system. The endocrine system is a group of glands and cells that make and release hormones into the blood, which control many functions such as growth, reproduction, sleep, hunger, and metabolism.
Structure
The pancreas is about 15 cm (6 inches) long. Its widest segment is called the head. Its narrowest part is called the tail. The middle section is called the body.
The pancreas has a series of small tubes that open into the pancreatic duct. The pancreatic duct joins with the common bile duct to drain into the duodenum. The duodenum is the first segment of the small intestine that receives partially digested food from the stomach, absorbs nutrients, and circulates digested food to the jejunum. The duodenum also receives bile (a greenish-yellow liquid that helps digest fat) from the liver and gallbladder.
Function of pancreas
The pancreas is made up of exocrine cells and endocrine cells. These cells have different functions.
Exocrine cells
Most of the cells in the pancreas are exocrine. They make and release pancreatic juice. This juice travels through the pancreatic duct to the duodenum. Enzymes found in pancreatic juice help digest fats, carbohydrates, and proteins in food.
Endocrine cells
A low number of cells in the pancreas are endocrine. They are grouped together in clusters called islets, or islets of Langerhans. These islets make and release insulin and glucagon into the blood. These hormones help control the level of sugar, or glucose, in the blood.
Insulin reduces the amount of sugar in the blood when blood sugar levels are high. It prompts the liver, muscles and fatty tissue to absorb and store excess sugar.
Glucagon increases the amount of sugar in the blood when blood sugar is low. It causes the liver and other tissues in the body to release stored sugar in the blood.

Cancerous tumors of the pancreas
A cancerous tumor of the pancreas can invade and destroy nearby tissue. It can also spread (metastasize) to other parts of the body. Cancerous tumor is also called a malignant tumor. About 95% of all cancerous pancreatic tumors start in exocrine cells. Exocrine cells make and release juices that aid digestion.
Ductal adenocarcinoma is the most common cancerous tumor of the pancreas. It accounts for about 95% of all pancreatic cancers. It affects 1.5 to 2 times more men than women, and it usually appears between the ages of 60 and 80.
Ductal carcinoma starts in the cells that line the ducts of the pancreas. Many ductal adenocarcinomas start in the head of the pancreas. They can also do it in the body or the tail of the pancreas.
Rare pancreatic tumors
The following cancerous pancreatic tumors are rare.
Adenosquamous carcinoma, also called adenoacanthoma, affects men 3 times more than women. It can appear at any age. It is treated with surgery, chemotherapy or radiotherapy.
Pancreatic neuroendocrine tumor (pNT) is more common in men than in women. It usually affects people over the age of 60. It appears in any part of the pancreas. It is treated with a combination of chemotherapeutic agents followed by surgery or radiotherapy.
Cystadenocarcinoma is somewhat more common in women than in men. It can appear at any age, but the average age at diagnosis is 48. This tumor mainly affects people without a history of pancreatitis (inflammation or infection of the pancreas). Cystadenocarcinoma is treated with surgery. Doctors have yet to decide what is the best type of surgery to perform since cystadenocarcinoma is so rare.
Acinar cell carcinoma affects men more than women. It can manifest at any age. This tumor can form lumps on the skin of the legs and then the arms, chest, abdomen and scalp. Acinar cell carcinoma can also cause arthritis, which causes pain when you move your joints but with little swelling. Acinar cell carcinoma is treated with surgery, chemotherapy or radiation therapy.
Polymorphic adenocarcinoma, also called giant cell carcinoma or sarcomatoid carcinoma, is slightly more common in men than in women. It mostly affects people in their 60s and the average age at diagnosis is 67 years. In rare cases, this tumor can cause jaundice. Polymorphic adenocarcinoma is treated with surgery, chemotherapy or radiation therapy.
Microadenocarcinoma tends to grow large and usually appears in the head or tail of the pancreas. The average age at diagnosis is 40 years old. Microadenocarcinoma is treated with surgery, chemotherapy or radiotherapy.
Pancreatoblastoma is most often seen in children. This tumor is removed by surgery.
Malignant oncocytoma is very rare. Since it is so rare, experts are unsure of the average age at diagnosis and whether it affects men more than women.
Lymphoma is a type of cancer that starts in lymphocytes, a type of white blood cell. It is very rare for a lymphoma to start in the pancreas. This is called primary lymphoma of the pancreas. It appears to affect men more than women, but the average age at diagnosis is 65. Treatment is based on the stage and specific type of tumor.
Sarcoma is a type of cancer that starts in connective tissue. It is very rare for a sarcoma to start in the pancreas. This is called primary sarcoma of the pancreas. Most pancreatic sarcomas are metastasized by sarcoma that started in the abdomen.
Precancerous conditions of the pancreas
Precancerous conditions of the pancreas are changes to the cells of the pancreas that make them more likely to become cancerous. These conditions are not yet cancerous, but the abnormal changes in cells could turn into pancreatic cancer if left untreated.
The most common precancerous conditions of the pancreas are these.
Mucinous cystic tumor (TKM) is observed in the body or tail of the pancreas. It most often affects women between the ages of 40 and 50.
Mucinous papillary intracanal tumor is usually seen in the head of the pancreas. It affects men and women, usually those in their sixties (60 years old) and those in their seventies (70 years old).
Solid pseudopapillary tumor (TPPS) most commonly appears in the tail of the pancreas. It is also known as Hamoudi’s tumor. It most commonly affects women in their twenties or thirties.
The neuroendocrine tumor can be precancerous or cancerous. The doctor looks at a sample of the tumor under a microscope to see if it is cancerous or not. Tumors that are more than 5 cm in diameter are usually cancerous. Sometimes the neuroendocrine tumor can produce excess hormones, especially insulin.
Symptoms of pancreatic cancer
The signs and symptoms of precancerous conditions of the pancreas include the following:
vague pain or discomfort in the abdomen
firm, unresponsive abdominal mass
yellowing of the skin and whites of the eyes (jaundice)
weightloss
symptoms of diabetes including unusual thirst, frequent urination, extreme fatigue or lack of energy, nervousness and sweating
Diagnostic
If you have any symptoms or if your doctor thinks you may have a precancerous condition of the pancreas, you will have tests. The tests that make it possible to diagnose precancerous conditions of the pancreas include the following:
an ultrasound, which might include endoscopy (EE)
a fine needle biopsy (FNB) guided by EE
computed tomography (CT)
endoscopic retrograde cholangiopancreatography (ERCP)
a magnetic resonance imaging (MRI) exam
Treatments
Surgery is usually used to treat precancerous conditions of the pancreas. Most precancerous conditions can be completely removed. The type of surgery done depends on the location of the tumor in the pancreas.
A distal pancreatectomy is used when the tumor is located in the body or tail of the pancreas. This surgery removes the tail of the pancreas, or the tail and part of the body of the pancreas, along with nearby lymph nodes. The spleen is only removed if the tumor has grown into the spleen or the blood vessels that supply it.
Whipple’s operation, also called a pancreatoduodenectomy, is used when the tumor is located in the head of the pancreas. This surgery removes the head of the pancreas as well as part of the duodenum (first segment of the small intestine), the gallbladder, part of the common bile duct, the pylorus (lower section of the stomach that is connected to the duodenum) and lymph nodes near the head of the pancreas.
Non-cancerous tumors of the pancreas
A non-cancerous (benign) tumor of the pancreas is a lump that does not spread to other parts of the body (not metastasize). The non-cancerous tumor is usually not life threatening. Usually, it’s removed by surgery and it doesn’t come back, or come back, usually not.
There are a few types of non-cancerous pancreatic tumors.
Pancreatic pseudocyst
A pancreatic pseudocyst is a sac of clear, or yellowish, watery fluid. This fluid has high amounts of pancreatic enzymes, including amylase, lipase and trypsin.
Pancreatic pseudocysts are more common in men than in women. Sometimes one pseudocyst develops. Sometimes many, or multiple, pseudocysts develop. About two-thirds of all pancreatic pseudocysts develop in the tail of the pancreas.
Pseudocysts are usually caused by injury to the pancreas or pancreatitis. Pancreatitis is inflammation or infection of the pancreas. It can be acute, which means it comes on suddenly and lasts a short time. It can also be chronic, which means it lasts a long time, but with milder symptoms compared to those caused by acute pancreatitis.
Pancreatic pseudocysts may go away on their own. If they cause pain or an infection develops, doctors will remove them.
Serous cystic neoplasm (SCN)
A serous cystic neoplasm (SCN) is a non-cancerous tumour that develops from glandular tissue. It is also called serous cystadenoma. Glandular tissue often makes and releases fluids. SCNs form when the fluids build up and form cysts.
SCNs are more common in women than in men. Most SCNs occur in the head and body of the pancreas.
SCNs rarely cause symptoms. If they do cause symptoms, such as pain, they are treated. They are usually removed with surgery.
Risk factors for pancreatic cancer
A risk factor is something, like a behavior, substance, or condition that increases the risk of developing cancer. Most cancers are caused by many risk factors, but sometimes pancreatic cancer develops in people who do not have any of the risk factors described below.
Precancerous conditions of the pancreas include mucinous cystic tumor (TKM) and intracanal papillary mucinous tumor (TIPM). These conditions are not cancerous, but they can turn into pancreatic cancer if left untreated. Certain risk factors for pancreatic cancer can also cause these precancerous conditions.
Risk factors are usually ranked from most important to least important. But in most cases, it is impossible to rank them with absolute certainty.
Known risk factors
There is convincing evidence that the following factors increase your risk for pancreatic cancer.
Tobacco
20-30% of pancreatic cancers are linked to smoking tobacco. The risk increases with the number of cigarettes and the number of years you smoke. The risk decreases as soon as you stop smoking. The longer the period after quitting smoking, the lower the risk of pancreatic cancer. Smoking cigars or pipes, or using smokeless tobacco products, such as chewing tobacco and snuff, also increases your risk of pancreatic cancer.
Obesity
People who are obese or have a high body mass index (BMI) are more likely to develop pancreatic cancer.
Diabetes
Pancreatic cancer occurs more often in people with diabetes, but it is not yet fully understood why. Perhaps obesity is a risk factor for both diabetes and pancreatic cancer, or diabetes could be an early sign of pancreatic cancer.
Family history of pancreatic cancer
About 10-20% of pancreatic cancers are hereditary, or familial, which means that several members of the family have it. In familial pancreatic cancer, at least 2 first-degree relatives (father, mother, brother, sister or child) or 3 family members have been diagnosed with pancreatic cancer. The risk of pancreatic cancer increases with the number of family members who have it. In some families, the increased risk may be due to an inherited genetic disorder. Others say doctors do not know what is causing the increase in the number of cases.
Certain genetic disorders
The following genetic disorders are linked to an increased risk of pancreatic cancer.
Hereditary breast and ovarian cancer is an inherited condition caused by changes (mutations) that have occurred in the BRCA1 or BRCA2 gene. People with inherited breast and ovarian cancer are at increased risk of breast, ovarian, prostate, pancreatic and fallopian tube cancer.
Dysplastic nevus syndrome (FAMMM) is an inherited condition that usually affects several members of a family. Melanoma and a large number of atypical moles (nevi) develop in family members who have FAMMM. Nevus are usually different sizes and colors. FAMMM is caused by a mutation in the p16 gene.
Peutz-Jeghers syndrome is an inherited syndrome that causes a large number of polyps to form in the digestive tract. It also causes black spots to appear on the lips and around and inside the mouth.
Lynch syndrome (also called hereditary nonpolyposis colorectal cancer, or HNPCC) is a rare inherited syndrome that can lead to colorectal cancer. A person with Lynch syndrome type B is more likely to get other cancers, including pancreatic cancer.
Hereditary pancreatitis is a rare genetic condition that causes severe pancreatitis at a young age, often before a child is 10 years old. Pancreatitis is the inflammation of the pancreas.
Multiple endocrine neoplasia type 1 (MEN 1) and von Hippel-Lindau disease are genetic disorders. They can increase your risk for neuroendocrine cancer of the pancreas (islet cancer).
Chronic pancreatitis
Chronic pancreatitis is the prolonged inflammation of the pancreas. People with this condition are more likely to get pancreatic cancer. Some studies also show a link between acute pancreatitis and pancreatic cancer. Acute pancreatitis is sudden, short-lived inflammation of the pancreas.
Red meat consumption
Studies have shown that eating red meat increases the risk of pancreatic cancer.
Possible risk factors
The following factors have been linked to pancreatic cancer, but there is not enough evidence to say that they are known risk factors. More research is needed to clarify the role of these factors in the development of pancreatic cancer.
Alcohol
According to some studies, excessive alcohol consumption may be linked to an increased risk of pancreatic cancer. This may be because excessive alcohol consumption is a common cause of chronic pancreatitis.
Physical inactivity
Research suggests that people who are physically active on a regular basis may be less likely to develop pancreatic cancer.
Consumption of processed meat
Several studies show a link between the consumption of processed meat and an increased risk of pancreatic cancer.
Occupational exposure to chemicals
Studies have shown that occupational exposure to certain chemicals for more than 10 years increases the risk of pancreatic cancer. These products are among others the following:
petroleum compounds and solvents
some dyes
chemicals required for refining
polycyclic aromatic hydrocarbons and chlorinated hydrocarbons
Helicobacter pylori
Helicobacter pylori (H. pylori) is a bacteria that thrives in the inner lining of the stomach. Some studies show a link between H. pylori infection and an increased risk of pancreatic cancer.
Hepatitis B virus
The hepatitis B virus (HBV) is a virus that causes infection in the liver. Some studies show that HBV infection increases the risk of pancreatic cancer.
Gum disease
Researchers are studying the possible links between gum disease (periodontal disease) and certain medical conditions. Some studies have shown that there is a link between gum disease, or the bacteria that causes it, and an increased risk of pancreatic cancer.
Cystic fibrosis
Cystic fibrosis is a genetic disease that affects the glands that produce mucus and sweat, which affects the function of the lungs and digestive tract. People with cystic fibrosis may be at higher risk for certain cancers, including pancreatic cancer, if they live with the disease for a long time.
Liver cirrhosis
Cirrhosis occurs when scar tissue replaces healthy tissue in the liver. Scar tissue blocks the flow of blood through the liver, preventing it from functioning normally. Cirrhosis is caused by long-term damage to liver tissue, such as drinking too much alcohol and or being infected with the hepatitis B or C virus. Research shows that cirrhosis increases the risk of breast cancer. liver, but it could also increase the risk of pancreatic cancer.
Unknown risk factors
It is not yet clear whether the following factors are linked to pancreatic cancer. This may be because researchers are unable to definitively establish this link, or the studies have yielded different results. More research is needed to find out if the following are risk factors for pancreatic cancer:
- surgery to remove the gallbladder (cholecystectomy)
- exposure to pesticides
Reduce the risk of pancreatic cancer
You can reduce your risk of pancreatic cancer by adopting the following behaviors.
Don’t smoke and avoid second-hand smoke
Smoking tobacco causes 20-30% of all pancreatic cancers. Not smoking is the best way to lower your risk of pancreatic cancer.
Live smoke-free. If you smoke, get help quitting. Do not consume any tobacco products, including chewing tobacco, cigars, cigarillos, and pipes. Avoid second-hand smoke.
Maintain a healthy weight
Studies have shown that obesity increases your risk of pancreatic cancer. You can reduce your risk by maintaining a healthy weight. Eating well and being physically active can help you maintain a healthy weight.
Limit your alcohol consumption
Some studies show that drinking too much alcohol may increase your risk of pancreatic cancer. Women who choose to drink alcohol should stick to less than 1 drink per day and men to less than 2 drinks per day. The less you drink, the more you reduce your risk.
Be physically active
Studies show that physical activity may reduce the risk of pancreatic cancer.
Limit your intake of red meat and processed meat
Studies show that eating lots of red meat and processed meat may increase your risk for pancreatic cancer.
Follow occupational health and safety requirements
Exposure to certain chemicals and certain jobs could increase your risk for pancreatic cancer. Follow occupational health and safety requirements when working with hazardous chemicals.
Find out if your risk of pancreatic cancer is high
Some people may have a higher than average risk of developing pancreatic cancer. Discuss your risk with your doctor. If it is above average, you may need a personalized screening plan.
Symptoms of pancreatic cancer
Pancreatic cancer may not cause any signs or symptoms in the very early stages of the disease. Signs and symptoms often appear when the tumor grows and causes changes in the body. Other medical conditions can cause the same symptoms as pancreatic cancer.
See your doctor if you have these signs or symptoms:
- yellowing of the skin and whites of the eyes (jaundice)
- pain in the upper abdomen or back
- fatty stools (steatorrhea) that are large and pale and that float in the toilet
- unexplained weight loss
- loss of appetite
- tired
- nausea and vomiting
- difficulty digesting
- feeling full after a light meal
- bloating
- gas
- diarrhea or constipation
- itching
- dark urine
- fever and tremors
- swelling of the legs
Diagnosis of pancreatic cancer
Diagnosis is the process of finding out the cause of a health problem. Diagnosing pancreatic cancer usually begins with a visit to your family doctor. Your doctor will ask you about any symptoms you have and do a physical exam. Based on this information, your doctor may refer you to a specialist or order tests to check for pancreatic cancer or other health problems.
The process of diagnosis may seem long and frustrating. It’s normal to worry, but try to remember that other health conditions can cause similar symptoms as pancreatic cancer. It’s important for the healthcare team to rule out other reasons for a health problem before making a diagnosis of pancreatic cancer.
The following tests may be used to rule out or diagnose pancreatic cancer. Many of the same tests used to diagnose cancer are used to find out the stage (how far the cancer has progressed). Your doctor may also order other tests to check your general health and to help plan your treatment.
Health history and physical exam
Your health history is a record of your symptoms, risk factors and all the medical events and problems you have had in the past. Your doctor will ask questions about your history of:
symptoms that suggest pancreatic cancer
smoking tobacco
obesity
diabetes
chronic pancreatitis (inflammation or infection of the pancreas)
Your doctor may also ask about a family history of:
pancreatic cancer
hereditary breast and ovarian cancer (HBOC) syndrome
familial atypical multiple mole melanoma (FAMMM) syndrome
Peutz-Jeghers syndrome
Lynch syndrome (also called hereditary non-polyposis colorectal cancer, or HNPCC)
hereditary pancreatitis
A physical exam allows your doctor to look for any signs of pancreatic cancer. During a physical exam, your doctor may:
check your skin and the whites of your eyes for jaundice
feel your abdomen for any lumps or swelling
feel your abdomen to see if your gallbladder, liver or spleen are larger than normal
check your legs for swelling
check the lymph nodes above your collarbone and in other places to see if they are swollen
Complete blood count (CBC)
A CBC measures the number and quality of white blood cells, red blood cells and platelets. A CBC is done to show how well the bone marrow and certain organs are functioning. It is also used to provide a baseline that your doctors can use to compare blood counts during and after treatment.
Blood chemistry tests
Blood chemistry tests measure certain chemicals in the blood. They show how well certain organs are functioning and can help find abnormalities. Blood chemistry tests may be used to measure the following chemicals:
bilirubin
alkaline phosphatase
lactic dehydrogenase (LDH)
alanine aminotransferase (ALT)
aspartate transaminase (AST)
amylase
An increased level of any
of these chemicals may indicate:
a blockage in the common bile duct or pancreatic duct
pancreatitis (inflammation or infection of the pancreas)
pancreatic cancer has spread to the liver
Tumour marker tests
Tumour markers are substances found in the blood, tissues or fluids removed from the body. An abnormal amount of a tumour marker may mean that a person has pancreatic cancer.
Tumour marker tests are generally used to check your response to cancer treatment. They can also be used to diagnose pancreatic cancer. These tests are not sensitive or specific enough to be used to screen for pancreatic cancer.
The following tumour markers may be measured for pancreatic cancer.
Carbohydrate antigen 19-9 (CA19-9) is a protein found in very small amounts on the surface of certain cancer cells. The level of CA19-9 is higher than normal in 70% to 80% of people with pancreatic cancer.
Carcinoembryonic antigen (CEA) is a protein normally found in the tissue of a developing fetus. Levels of CEA in the blood decrease after birth. The level of CEA is higher than normal in about 50% of people with pancreatic cancer.
Find about more about tumour marker tests.
CT scan
A computed tomography (CT) scan uses special x-ray equipment to make 3-D and cross-sectional images of organs, tissues, bones and blood vessels inside the body. A computer turns the images into detailed pictures.
A CT scan is the most common imaging test for pancreatic cancer. It is used to:
find tumours
find out the size of the tumour
find out if the tumour can be completely removed with surgery
find out if the cancer has spread to nearby organs and tissues
guide a fine needle aspiration (FNA) biopsy to get tissue samples
Ultrasound
An ultrasound uses high-frequency sound waves to make images of parts of the body. It is used to:
- find tumours
- help tell different types of tumours apart
- guide a fine needle aspiration (FNA) biopsy to get tissue samples
An abdominal ultrasound may be one of the first tests done if you have unexplained abdominal pain. It can also be used to look at the liver.
An endoscopic ultrasound (EUS) is a newer procedure that can diagnose pancreatic cancer more accurately than an abdominal ultrasound. An endoscope is a thin, tube-like instrument with a light and lens on the end. During an EUS, the doctor passes an endoscope down the throat, through the esophagus and stomach, and into the duodenum (first part of the small intestine). The doctor then passes an ultrasound probe down the endoscope and points it toward the pancreas. An ultrasound scan is taken of the pancreas and nearby organs.
An EUS creates a very accurate picture and is good for finding small tumours. Doctors can also collect a tissue sample for a biopsy during an EUS.
MRI
Magnetic resonance imaging (MRI) uses powerful magnetic forces and radiofrequency waves to make cross-sectional images of organs, tissues, bones and blood vessels. A computer turns the images into 3-D pictures.
An MRI is used to find tumours and check to see if the cancer has spread to other organs and tissues.
Magnetic resonance cholangiopancreatography (MRCP) is a special type of MRI that produces detailed pictures of the liver, gallbladder, bile ducts, pancreas and pancreatic duct.
Endoscopic retrograde cholangiopancreatography (ERCP)
An ERCP is similar to an endoscopic ultrasound. It is a procedure that uses an endoscope (a thin, tube-like instrument with a light and lens on the end) and x-rays to examine the ducts that drain the pancreas, liver and gallbladder. A dye is injected into the ducts to make them show up clearly on an x-ray. X-rays are taken as soon as the dye is injected.
ERCP is used to:
find a tumour that may be causing a blockage in the bile duct or pancreatic duct
collect a sample for biopsy
place a tube (stent) to relieve the blockage of the bile duct
Laparoscopy
A laparoscopy is a procedure in which an endoscope (a thin, tube-like instrument with a light and lens on the end) is passed through a small cut (incision) in the abdomen. Using a laparoscopy can help avoid the need for more extensive abdominal surgery.
Laparoscopy is used to:
look at the pancreas and surrounding areas
collect a tissue sample for a biopsy
Biopsy
During a biopsy, the doctor removes tissues or cells from the body so they can be tested in a lab. A report from the pathologist will show whether or not cancer cells are found in the sample.
Fine needle aspiration (FNA) is the type of biopsy used to collect a sample from the pancreas. An FNA uses a thin needle and a syringe to remove a small amount of fluid or cells.
An FNA of the pancreas can be done through the skin. The doctor uses a CT scan or an ultrasound to guide the needle to the tumour. An FNA can be done during a laparoscopy, an EUS or an ERCP.
An FNA may also be used to collect samples from the liver to see if cancer has spread to the liver.
PET scan
A positron emission tomography (PET) scan uses radioactive materials called radiopharmaceuticals to look for changes in the metabolic activity of body tissues. A computer analyzes the radioactive patterns and makes 3-D colour images of the area being scanned.
A PET scan is used to:
find tumours
find out if cancer has spread to other organs and tissues
Percutaneous transhepatic cholangiography (PTC)
A PTC is an x-ray of the bile ducts and liver. The doctor inserts a thin needle through the skin into the bile duct area. A contrast medium, or special dye, is injected into the bile ducts. The dye outlines the structure of the bile ducts and liver on the x-ray.
A PTC may be used to find out if there is a blockage in the bile duct. Doctors may also use a PTC to guide them as they place a stent to open a blocked bile duct.
Histological classification of pancreatic cancer (grading)
The grade is defined by the appearance of cancer cells compared to normal cells. To establish the grade of pancreatic cancer, the pathologist examines a sample of tissue taken from the tumor under a microscope. The pathologist assigns a grade of 1 to 4 to pancreatic cancer. The lower this number, the lower the rank.
The term differentiation is used to refer to how different cancer cells are.
Low-grade cancer cells are well differentiated. They almost look like normal cells. They tend to grow slowly and are less likely to spread.
High-grade cancer cells are poorly differentiated or undifferentiated. Their appearance is less normal, or more abnormal. They tend to grow faster than low grade cancer cells.
Knowing the grade gives your healthcare team an idea of how quickly cancer can grow and how likely it is to spread. It helps him plan your treatment. The grade can also help the healthcare team determine the possible outcome of the disease (prognosis) and predict how the cancer might respond to treatment.
Stages of pancreatic cancer
Staging describes or categorizes cancer based on how much cancer is in the body and where it was initially diagnosed. This is often referred to as the extent of cancer. Information from tests is used to find out how big the tumor is, what parts of the organ have cancer, if the cancer has spread from where it started and where it has spread. Your healthcare team uses the stage to plan your treatment and predict the outcome (your prognosis).
One of the frequently used staging systems for pancreatic cancer is the TNM classification. Often, doctors also use a simple clinical staging system based on the ability to remove pancreatic cancer by surgery (resectability).
Can the tumor be removed by surgery?
Despite the sophisticated tests used to diagnose pancreatic cancer, doctors cannot always know the exact size of the tumor and how far it has spread before having the surgery. This is why doctors often divide pancreatic cancers into groups based on resectability.
Resectable
A tumor is resectable when it can be completely removed with surgery. Cancer is resectable when the tumor:
is only present in the pancreas and has not spread to other parts of the body (distant metastasis);
does not affect the superior mesenteric vein (MSV) or the portal vein;
does not affect the celiac artery, hepatic artery or superior mesenteric artery (MSA).
At the limit of resectability
A tumor is borderline resectable when it has spread into a large blood vessel, but it would still be possible to remove it and rebuild the blood vessel. Cancer is borderline resectable when the tumor:
has not spread to other parts of the body, that is, there is no distant metastasis;
touches or leans on the MSV or portal vein, but that doctors may be able to safely remove the tumor and reconstruct the vein;
is very close to or touches the hepatic artery, but does not extend to the celiac artery;
is very close to AMS or touches it, but that it does not invade it.
Unresectable
A tumor is unresectable when it cannot be completely removed with surgery. This may be because the cancer is locally advanced or metastatic.
Locally advanced means that the cancer has spread too far into the blood vessels or other nearby tissue to be completely removed, but it has not spread to distant organs or tissues.
Metastatic means the cancer has spread to distant organs.
TNM classification
In the case of pancreatic cancer, the TNM classification has 5 stages, ie stage 0 followed by stages 1 to 4. For stages 1 to 4, the Roman numerals I, II, III and IV are often used. But in order to make the text clearer, we will use the Arabic numerals 1, 2, 3 and 4. In general, the higher the stage number, the more cancer has spread. Talk to your doctor if you have questions about staging.
Stage 0 (or carcinoma in situ)
Cancer cells are seen only in the lining of the pancreas.
Stage 1
The tumor is 4 cm or less. In stage 1A, the tumor is 2 cm or less. In stage 1B, the tumor measures more than 2 cm but not more than 4 cm.
Stage 2
The tumor is over 4 cm (stage 2A) or the tumor is any size and the cancer has spread to 1 to 3 nearby lymph nodes (stage 2B).
Stage 3
The cancer has spread to at least 4 nearby lymph nodes or the tumor has grown to large blood vessels outside the pancreas and the cancer may have spread to nearby lymph nodes.
Stage 4
The cancer has spread to other parts of the body, such as the liver, lungs or abdominal cavity. We can also say that it is metastatic cancer of the pancreas.
Recurrence of pancreatic cancer
Recurrence of pancreatic cancer means that the cancer comes back after treatment. If it reappears where it first started, it is called a local recurrence. If it reappears in tissues or lymph nodes near where it first started, it is called a regional recurrence. It can also reappear in another part of the body: this is called a recurrence or distant metastasis.
If pancreatic cancer spreads
Cancer cells can spread from the pancreas to other parts of the body. This spread is called metastasis.
Understanding how a type of cancer usually grows and spreads helps your healthcare team plan for your treatment and future care. If pancreatic cancer spreads, it can spread to the following parts of the body:
- nearby lymph nodes
- bile ducts
- missed
- peritoneum (lining of the abdomen)
- liver
- lungs
- bone
Prognosis and survival for pancreatic cancer
If you have pancreatic cancer, you may be wondering about your prognosis. A prognosis is the act by which the doctor best assesses how cancer will affect a person and how they will respond to treatment. The prognosis and survival depend on many factors. Only a doctor who is familiar with your health history, the type of cancer you have, the stage and other characteristics of the disease, the treatments chosen and the response to the treatment can review all of this data together with the statistics of. survival to arrive at a prognosis.
A prognostic factor is an aspect of the cancer or a characteristic of the person, such as smoking, that the doctor considers when making a prognosis. A predictor factor influences how cancer responds to a certain treatment. Prognostic and predictor factors are often discussed together and both play a role in choosing a treatment plan and establishing the prognosis.
The following are the prognostic factors for pancreatic cancer:
Resectability
Resectability is the ability to completely remove the tumor with surgery. It is one of the most important prognostic factors for pancreatic cancer. The prognosis is better when the tumor can be completely removed by surgery, that is, it is resectable.
Stadium
Another important prognostic factor for pancreatic cancer is the stage, which indicates where the cancer is in the body. In general, the prognosis is better if the cancer is detected early and if its stage is low.
Functional index
The Functional Index is a measure of a person’s ability to perform routine tasks as well as their daily activities. It is often assessed on the Karnofsky Functional Index scale. People with a high functional index (Karnofsky index greater than 70) before surgery have a better prognosis than those with a low functional index.
Grade
Low grade pancreatic cancer has a better prognosis than high grade pancreatic cancer.
Survival
Survival is the probability of surviving cancer in the absence of other causes of death. It is used to estimate the percentage of people who will survive their cancer.
Most of the time, survival after 5 years for pancreatic cancer is 8%, which means that about 8% of people diagnosed with pancreatic cancer will survive at least 5 years.
Survival by stage
Survival varies depending on the stage of pancreatic cancer.
Pancreatic cancer usually progresses quickly and has a poor prognosis.
In general, the earlier you diagnose and treat pancreatic cancer, the better the prognosis.
Often, pancreatic cancer is not detected until at an advanced stage, after the tumor has spread or cannot be removed by surgery, which may make it a little more difficult to remove. treat.
Pancreatic cancer often comes back after treatment (comes back), even after being completely removed by surgery.
Survival by stage for pancreatic cancer is recorded as observed survival after 5 years. Observed survival is the percentage of people with a particular type of cancer who are still living to a specific time. Since observed survival does not take into account the cause of death, people who are no longer alive 5 years after their diagnosis may have died of cancer or another cause.
Treatments for pancreatic cancer
If you have pancreatic cancer, your healthcare team will make a treatment plan just for you. It will be based on your health and specific cancer information. When your healthcare team decides what treatments to offer for pancreatic cancer, they take into account the size and location of the tumor and your overall health.
The stage of the cancer, including whether the tumor is resectable, bordering on resectability or unresectable (locally advanced or metastatic), determines which treatments can be offered.
Pancreatic tumors that are resectable can be removed completely with surgery. Stage 1 or 2 tumors are often resectable. They are treated with surgery to remove part or all of the pancreas. Chemotherapy may be given after surgery (adjuvant chemotherapy). If cancer cells are seen in the tissue removed with the tumor during surgery, that is, the surgical margins are positive, then radiation or chemoradiation therapy can be given.
Pancreatic tumors that are borderline resectable are treated, if possible, in clinical trials. They could be treated before surgery with chemotherapy and chemoradiotherapy (neoadjuvant treatments).
Locally advanced pancreatic tumors (stage 3) are treated with chemotherapy, radiotherapy or chemoradiotherapy. In some cases, surgery is done to relieve symptoms of advanced cancer, called palliative surgery, but it is not done to try to remove all of the tumor.
Metastatic pancreatic tumors (stage 4) are treated with chemotherapy, with or without targeted therapy. You may be offered surgery, radiation therapy, or both to relieve symptoms and control pain, or palliative treatment.
You may be offered one or more of the following treatments for pancreatic cancer.
Surgery
Depending on the stage, size and location of the tumor, you may have one of the following types of surgery.
Whipple’s operation, also called a pancreatoduodenectomy, is used to remove tumors in the head of the pancreas or in the opening of the pancreatic duct. The head of the pancreas is removed as well as the duodenum (first segment of the small intestine), the gallbladder, part of the common bile duct, the pylorus (lower section of the stomach that connects to the duodenum) and the lymph nodes located near the head of the pancreas.
You can also do a modified Whipple’s operation, also called a pancreatoduodenectomy with conservation of the pylorus, to remove tumors in the head of the pancreas that are not large, or bulky, and that have not spread to the duodenum or spread to the lymph nodes. lymphatics surrounding the pylorus. It’s a modified version of Whipple’s surgery that does not remove the pylorus. Since the modified Whipple operation does not affect the normal functioning of the stomach, possible nutritional problems are avoided after the Whipple operation.
Distal pancreatectomy is used to remove tumors located in the body or tail of the pancreas. The tail of the pancreas, or the tail and part of the body of the pancreas, is removed, as well as the nearby lymph nodes. The spleen is only removed if the tumor has spread to the spleen or to the blood vessels supplying the spleen. A distal pancreatectomy is not often used because cancer that started in the body or tail of the pancreas has often spread by the time it is diagnosed.
A total pancreatectomy is done, only if necessary, to completely remove the tumor. It is very difficult to recover from this surgery, which is why it is not used as often as the Whipple operation or the modified Whipple operation. Total pancreatectomy removes the entire pancreas as well as the duodenum, pylorus, part of the common bile duct, gallbladder, sometimes the spleen and nearby lymph nodes.
Palliative surgery is used to relieve symptoms of advanced cancer. The types of surgeries that are possible are stent placement and surgical bypass. These procedures can help clear a blockage in the common bile duct or duodenum.
Chemotherapy
In chemotherapy, anti-cancer drugs (cytotoxics) are used to destroy cancer cells. Some chemotherapy drugs are given on their own. But it happens more often that we combine several.
The most common chemotherapy drugs used to treat pancreatic cancer include:
gemcitabine (Gemzar)
5-fluorouracil (Adrucil, 5-FU)
nab-paclitaxel (Abraxane)
FOLFIRINOX – folinic acid (leucovorin), irinotecan (Camptosar), oxaliplatin (Eloxatin) and 5-fluorouracil
Find out more about chemotherapy.
Radiotherapy
In radiation therapy, high-energy rays or particles, such as x-rays and gamma rays, are used to destroy cancer cells.
Pancreatic cancer is usually treated with external beam radiation therapy. A device emits the radiation through the skin to the tumor and some of the surrounding tissue.
Chemoradiotherapy
Chemoradiotherapy combines chemotherapy with radiotherapy. Both are administered during the same period. Certain types of chemotherapy make radiation therapy more effective.
If you cannot or do not want to be treated for cancer
You may want to consider care that aims to make you feel better without treating the cancer itself, perhaps because cancer treatments no longer work, are no longer likely to improve your condition, or their side effects are difficult to tolerate. There may be other reasons why you cannot or do not want to be treated for cancer.
Talk to members of your healthcare team. They can help you choose the care and treatment for advanced cancer.
Monitoring
Follow-up after treatment is an important part of caring for people with cancer. You will need to have regular follow-up visits, especially during the first 2 to 3 years after treatment. These visits allow the healthcare team to monitor your progress and to know how you are recovering from treatment.
Clinical tests
A few clinical trials in pancreatic cancer are underway in certain countries and are accepting participants. Clinical trials aim to find new methods of preventing, detecting and treating cancer.
Follow-up after treatment for pancreatic cancer
Follow-up after treatment for pancreatic cancer is an important part of the care of people with cancer. Cancer specialists and your family doctor often share this responsibility. Your healthcare team will talk to you to decide which follow-up meets your needs.
Don’t wait until your next scheduled appointment to report any new symptoms and any symptoms that don’t go away. Notify your healthcare team if:
- you have pain in your upper abdomen or back;
- you have lost weight;
- your skin and the whites of your eyes are yellowish (jaundice);
- you are itchy;
- your digestion has changed (difficulty digesting, nausea and vomiting for example);
- you’ve lost your appetite.
The risk of pancreatic cancer coming back (recurring) is higher in the first 2 to 3 years after treatment, so close monitoring is necessary during this time.
Planning of follow-up visits
Pancreatic cancer follow-up visits are scheduled according to your personal needs. These visits after surgery are usually scheduled as follows:
- every 3 to 6 months for the first 3 years after treatment
- every 6 to 12 months for the next 2 years
- once a year thereafter
Conduct of follow-up visits
During a follow-up visit, your healthcare team will usually ask you questions about the side effects of treatment and how well you are coping. You may also be asked if you are in pain, and you may be helped if you are having difficulty eating and experiencing eating disorders.
Your doctor may do a physical exam including:
- feel your abdomen;
- feel your lymph nodes.
Examinations may also be ordered as part of the follow-up.
If your healthcare team finds out that the cancer has come back, they will talk to you to plan your treatment and care.
View this post on Instagram
Supportive care for pancreatic cancer
Supportive care empowers people to overcome the physical, practical, emotional and spiritual barriers of pancreatic cancer. It is an important component of the care of people with this disease. There are many programs and services that help meet the needs and improve the quality of life for these people and their loved ones, especially after treatment is over.
Recovering from pancreatic cancer and adjusting to life after treatment is different for everyone, depending on the location of the cancer, the stage of the cancer, the tissues and organs removed during the surgery, the type of treatment and much more. other factors. The end of cancer treatment can lead to mixed emotions. Even if the treatment is finished, there may be other issues that need to be addressed, such as coping with long-term side effects. A person who has been treated for pancreatic cancer may be concerned about the following.
Self-esteem and body image
Self-esteem is how we feel about ourselves. Body image is how we perceive our own body. Pancreatic cancer and its treatments can affect self-esteem and body image. This is often because cancer or cancer treatments cause changes in the body such as the following:
- scars
- hair loss
- skin changes
- changes in body weight
Some of these changes may be temporary, others will last a long time, and some will be permanent.
For many people, body image and how other people look is closely related to self-esteem and can be a source of real concern and significant distress. They may be afraid to go out or fear being rejected by others, or be angry or upset, even though the effects of treatment may not be visible.
Pain
Pain in pancreatic cancer is most often due to the location of the tumor and its effect on other structures (such as nearby tissues, nerves, blood vessels, bile and pancreatic ducts, or other organs. ) as the cancer progresses. A person may also experience pain following surgery for pancreatic cancer.
Treating pain is an important part of improving the quality of life for someone with pancreatic cancer. The pain associated with pancreatic cancer can be treated in several ways.
Pain relievers are frequently used to treat pain associated with pancreatic cancer. Your doctor will decide which type of painkiller and what dose is best for you. Opioids like morphine are the most common type of painkiller. Special drugs are also given to treat nerve pain.
Pain relievers are administered at a fixed schedule either by mouth (oral route), by injection, by a patch applied to the skin (transdermal) or by a needle inserted into a vein (intravenous route). Many pain relievers cause side effects such as constipation and nausea. Your doctor may prescribe softeners or laxatives and anti-nausea medications to help prevent these side effects.
A nerve block can be done to treat pain caused by a damaged nerve. The solar plexus is a mass of nerves located at the back of the abdomen. Pancreatic cancer can cause pain if it affects these nerves. In solar plexus nerve blockage, local anesthetic and drugs are injected into the solar plexus to numb the nerves.
Surgery may be used to treat pain caused by a blockage in a bile duct or duodenum. A tube (stent) is inserted into the bile duct or duodenum to keep it open. You can also do surgery to get around a blockage.
Radiation therapy given alone or in combination with chemotherapy can also help control pain. These treatments can reduce the size of a tumor that puts pressure on a nerve or other organ, causing pain.
Physiotherapy, psychotherapy and complementary treatments can also be used to control the pain. We are therefore talking about massage therapy, relaxation and deep breathing.
Nutritional disorders
Often people with pancreatic cancer have nutritional problems. You may not be able to digest fat if you have your pancreas or if it is not working properly or if a bile or pancreatic duct is blocked. This blockage can be treated by inserting a stent into the canal to keep it open. You may also be given pancreatic enzymes to aid digestion. Medicines like steroids can help increase your appetite.
Eating well during cancer treatment is important, so talk to your healthcare team if you have any of the following issues.
Nausea and vomiting
Nausea and vomiting are common side effects of treatment for pancreatic cancer. There are ways to prevent and treat nausea and vomiting.
Weightloss
When the pancreas is not working properly, or a bile or pancreatic duct is blocked, not enough bile and digestive enzymes are released in the small intestine. Pancreatic cancer can also release cytokines into the blood. Cytokines change the way the body uses nutrients and can cause the body to burn calories faster than it replaces them.
These problems can lead to weight loss and fatigue, which can greatly affect your quality of life, your ability to carry out daily activities and your response to treatment. It is important that you maintain your weight even if your appetite has changed. Proper nutrition helps the body fight disease and cope with the effects of treatment for pancreatic cancer.
Diarrhea
If you have pancreatic cancer, you may have different types of diarrhea. In some people with blocked bile ducts, stools may be the color of clay. If the pancreas does not make enough enzymes to help the gut digest food and absorb nutrients, the stool may float.
Changing your diet somewhat can help relieve diarrhea. One of the most important things to do in treating diarrhea is to drink enough fluids to stay hydrated.
Your doctor may prescribe vitamin supplements if your stool is loose because your gut is not absorbing nutrients well enough, which is called malabsorption. You should try to avoid foods that are high in fat, greasy, or fried as you may have difficulty digesting them.
Loss of appetite
Loss of appetite is common in people with pancreatic cancer. It can be caused by surgery, medication, taste changes, or even cancer.
Your healthcare team can help you cope with loss of appetite and increase your interest in food and your appetite.
Insufficient pancreatic enzymes
Pancreatic enzymes help the body digest food by breaking down fats, proteins, and carbohydrates. Often, people with pancreatic cancer do not have enough pancreatic enzymes to break down food, which means their gut cannot absorb the nutrients from food. The most common side effect of insufficient pancreatic enzymes is constipation.
Your doctor may prescribe digestive enzymes to help improve digestion and absorption of food. Take digestive enzymes with every meal or snack that contains fat, especially meat, dairy products, bread, and desserts. For best results, take enzymes before eating and throughout the meal.
Tired
Fatigue makes a person feel more tired than usual and can interfere with daily activities and sleep. Many people with pancreatic cancer experience fatigue from the disease or its treatment. Fatigue can be caused by anemia, specific medications, depression, or toxic substances that are produced when cancer cells break down and die. Pancreatic cancer often causes nutritional problems, which can make fatigue worse. It can be difficult to cope with the situation when you feel very tired and don’t have a lot of energy.
Diabetes
You may have diabetes if you have some or all of your pancreas removed because it makes less insulin. You will need to take insulin to help regulate your blood sugar levels. You should also so learn to check your blood sugar.
Hunting syndrome
Hunting syndrome is a collection of symptoms that occurs when food passes too quickly from the stomach to the small intestine. This syndrome can appear after surgery for pancreatic cancer. Sometimes it occurs right after a meal or up to 3 hours later. Symptoms include the following:
bloating
cramps
vomiting
diarrhea
sweat
Treatment includes dietary changes, medication, and surgery.
Jaundice
Most people with pancreatic cancer will have jaundice. It is caused by blockage of a bile duct or damage to the liver. Symptoms of jaundice include the following:
yellowing of the skin and whites of the eyes
dark yellow urine
clay colored stool
very dry skin that itches extremely
Skin problems caused by jaundice can be relieved by using anti-itch medications and oil-based or anti-itch creams. You can also use a mild soap and take baths to which you add baking soda.
Surgery can be done to clear a blocked bile duct. It allows a stent to be placed to keep the canal open or to bypass the blockage. These procedures allow bile to flow around the blockage and ease the jaundice.
Bowel obstruction
Bowel obstruction (blockage) occurs when the large or small intestine becomes blocked and the contents fail to pass. Blockage can be caused by:
a tumor of the pancreas that spreads or puts pressure on the intestine;
certain drugs that affect the digestive tract, such as painkillers and anti-diarrhea drugs.
The symptoms are among others:
abdominal pain
swelling of the abdomen
nausea
vomiting
constipation
diarrhea
Bowel obstruction can be treated with resting the bowel or with surgery. If you need to take opioid painkillers, your healthcare team will talk to you about a bowel elimination regimen that aims to prevent bowel obstruction. This regimen includes the regular use of laxatives.
Ascites
Ascites is the abnormal buildup of fluid in the abdomen that occurs with certain cancers. Symptoms of ascites include the following:
- swelling of the abdomen
- abdominal discomfort
- shortness of breath
- weight gain
- nausea
- vomiting
Paracentesis is usually done to relieve ascites. During paracentesis, a fine needle or tube is inserted through the skin into the abdominal cavity to remove the fluid. Sometimes chemotherapy is given to relieve ascites. Find out more about chemotherapy.
List of all Cancers
The word “cancer” is a generic term for a large group of diseases that can affect any part of the body. We also speak of malignant tumors or neoplasms. One of the hallmarks of cancer is the rapid multiplication of abnormal growing cells, which can invade nearby parts of the body and then migrate to other organs. This is called metastasis, which is the main cause of death from cancer. Types of cancer (in alphabetical order of the area concerned):
Information: Cleverly Smart is not a substitute for a doctor. Always consult a doctor to treat your health condition.
Sources: PinterPandai, American Cancer Society, Web MD, Cancer Center, Cleveland Clinic
Photo credit: Wikimedia Commons
Photo descriptions: cancerous cells forming a lump in the pancreatic tissue.