Tropical Diseases
Infectious and Tropical Diseases includes doctors specializing in all areas of infectious diseases, more particularly infections of the immunocompromised (weakened immune system), traveler and migrant and emerging infections as well as HIV infection, tuberculosis, leprosy, sexually infections, transmissible diseases, clinical viral infections, infectious skin diseases, vulvar pathology, parasitology and tropical diseases.
Tropical diseases are diseases that are found almost exclusively in countries between the Tropic of Cancer and the Tropic of Capricorn. These are the majority of countries in Asia, Central and Latin America, as well as Africa. This article tells you all about these pathologies and how to protect yourself from them!
Summary
- Tropical diseases: infection and transmission
- The risk of tropical diseases from mosquitoes
- The risk of tropical diseases from contaminated water and food
- Tropical diseases transmitted by insects
- Tropical diseases: other risks
Tropical diseases: infection and transmission
The climate, poorer hygiene conditions and more difficult access to healthcare explain the proliferation of tropical diseases in these regions. Some actors of disease transmission, such as mosquitoes or certain parasites, can only survive in a hot or very humid climate.
Infection with these diseases is very rare in France and in Western countries. The risk concerns those who live or stay in a tropical country (tourists, expatriates, migrants). When traveling to a tropical country, good preparation and simple rules to follow on site can prevent the risk of tropical diseases.
Since 2010, the World Health Organization has focused on 17 neglected tropical diseases that affect around 1 billion people in developing countries and that would require more investment, such as dengue, rabies, Chagas disease, leprosy or Buruli ulcer…
The risk of tropical diseases from mosquitoes
Tropical mosquitoes can transmit several infectious diseases, the best known of which is malaria.
Malaria
Malaria is an infectious disease caused by a parasite transmitted by mosquitoes, which stings especially at nightfall.
The symptoms are fever, headache, vomiting, and in extreme cases a coma.
It is preventable by using mosquito repellents and wearing long clothes, especially at nightfall; and taking preventive treatment, which varies according to the region of the world visited.
The dengue
Dengue fever is a viral disease (an arbovirus) transmitted by Aedes mosquitoes, which bite during the day. It is less fatal than malaria and is only complicated in 1% of cases.
Symptoms of dengue fever are fever, pain behind the eyes, vomiting, anorexia, joint and muscle pain, a red rash on the skin. Usually the illness lasts 5 days
It can become complicated and lead to severe forms (especially in children):
- haemorrhagic (cutaneous haemorrhages, epistaxis, digestive haemorrhages requiring transfusion);
- hepatic cells ranging from a transient benign elevation of transaminases with hepatomegaly or jaundice to acute fatal hepatic failure;
- shock with bleeding disorders causing diffuse bleeding.
Rare, it is prevented by the use of mosquito repellents.
Chikungunya
Typical symptoms of chikungunya are fever, severe muscle and joint pain, and a rash in the form of spots. Generally, this tropical disease, which is found in Southeast Asia, Africa and the Arabian Peninsula, goes away on its own. In rare cases, joint pain can last for months or even years.
Chikungunya is a viral disease transmitted to humans by infected mosquitoes. It is caused by the chikungunya virus (CHIKV).
CHIKV infection causes fever and severe joint pain. Other possible symptoms include muscle pain, joint swelling, headache, nausea, fatigue, and rash.
Joint pain is often debilitating and of varying duration.
There is currently no vaccine or specific drug against this virus. Treatment is primarily aimed at relieving symptoms.
The disease is mainly present in Africa, Asia and the Indian subcontinent. However, a large-scale outbreak occurred in several countries in the Region of the Americas in 2015 and sporadic outbreaks are observed in other regions.
Some clinical signs of chikungunya are the same as those of dengue fever and Zika virus disease, which can lead to misdiagnosis in areas where these diseases coexist.
Severe or fatal cases of chikungunya are very rare, and are almost always associated with the existence of other conditions.
Given the difficulties in making an accurate diagnosis of chikungunya, there is no real estimate of the number of people affected by the disease each year worldwide.
The presence of breeding sites near human dwellings is an important risk factor for chikungunya.
Yellow fever
Yellow fever is an acute viral hemorrhagic disease transmitted by infected mosquitoes. The term “yellow” refers to the jaundice presented by some patients.
The symptoms are: fever, headache, jaundice, myalgia, nausea, vomiting and fatigue.
In a small proportion of cases, patients contracting the disease develop severe symptoms, and about half of them die within 7 to 10 days.
The virus is endemic in the tropics of Africa, Central America and South America.
Large outbreaks of yellow fever occur when infected individuals introduce the virus to densely populated areas with a high density of mosquitoes and where most people have little or no immunization due to inadequate vaccination. Under these conditions, infected mosquitoes pass the virus from person to person.
Prevention of yellow fever is possible with an extremely effective, safe and inexpensive vaccine. A single dose of it confers long-lasting immunity and provides lifelong protection against disease, without the need for a booster dose. The vaccine confers effective immunity within 30 days for 99% of vaccinees.
Good symptomatic treatment in a hospital setting improves survival rates. There are currently no specific antiviral drugs for yellow fever.
The Eliminate Yellow fever Epidemics (EYE) strategy launched in 2017 is an unprecedented initiative. With the participation of more than 50 partners, this EYE partnership is helping 40 at-risk countries in Africa and the Americas with prevention, diagnosis and response to suspected cases and outbreaks of yellow fever. By 2026, more than one billion people are expected to be protected against the disease.
Dengue and severe dengue
Dengue is a mosquito-borne viral infection that plagues the tropics and subtropics around the world, with a predilection for urban and semi-urban areas.
The virus responsible for the disease is the dengue fever virus (DENV). There are four serotypes, which means you can be infected four times.
Although many DENV infections have mild manifestations, DENV can cause acute flu-like illness. Sometimes life-threatening complications arise. We then speak of severe dengue.
Severe dengue is one of the leading serious illnesses and causes of death in some countries in Asia and Latin America. It must be taken care of by a doctor.
There is no specific treatment for dengue or severe dengue. Early detection of signs of progression to severe dengue and access to appropriate medical care can reduce the death rate from severe dengue to less than 1%.
The worldwide incidence of dengue has increased dramatically in recent decades. About half of the world’s population is at risk. Although there are an estimated 100 to 400 million infections each year, more than 80% of them are usually mild and asymptomatic.
The fight against dengue is based on effective vectorial measures. Sustained community participation can make vector control much more effective.
Dengue fever is a mosquito-borne viral disease that has spread rapidly in all WHO regions in recent years. The virus is transmitted to humans through the bite of infected female mosquitoes, mainly of the species Aedes aegypti, but also of Ae. albopictus, to a lesser extent. These mosquitoes are also vectors of the chikungunya virus, the yellow fever virus and the Zika virus. Dengue fever is widespread in the tropics, with local variations in risk mainly depending on precipitation, temperature, relative humidity and rapid and uncontrolled urbanization.
Dengue has a wide range of symptoms, which can range from subclinical manifestations (people may not always know they are infected) to severe flu-like symptoms. Although it is less common, some people have severe dengue, a form of the disease that causes a number of complications related to severe bleeding, organ failure and / or plasma leakage. In severe dengue fever, the risk of death is higher if the treatment is not appropriate. Severe dengue was first described in the 1950s, during epidemics in the Philippines and Thailand. Today, the countries of Asia and Latin America are the most affected and it has become a major cause of hospitalization and death for children and adults in these regions.
Dengue fever is caused by a virus of the Flaviviridae family, of which there are four closely related serotypes (DENV-1, DENV-2, DENV-3 and DENV-4). Recovery is believed to result in lifelong immunity to the serotype causing the infection. In contrast, cross-immunity to other serotypes after recovery is only partial and temporary. Subsequent (secondary) infections with other serotypes increase the risk of developing severe dengue.
Zika (virus disease)
Zika virus disease is caused by a virus transmitted mainly by mosquitoes of the genus Aedes.
Affected subjects may present with moderate fever, rash (exanthema), conjunctivitis, muscle and joint pain, malaise, or headache. Normally, these symptoms go away in 2 to 7 days.
There is scientific consensus that the Zika virus is the cause of microcephaly and Guillain-Barré syndrome. Links to other neurological complications are under investigation.
The length of incubation period (from time of exposure to onset of symptoms) is not well known, but it is likely to be a few days. Symptoms resemble those of other arboviruses, such as dengue fever, and include fever, rash, conjunctivitis, muscle and joint pain, malaise, and headache. They usually remain benign and disappear within 2 to 7 days.
Zika virus disease is usually relatively mild and does not require specific treatment. Affected people need plenty of rest, enough drink, and common pain and fever medications. If symptoms worsen, they should see a doctor. There is currently no vaccine.
West Nile fever
West Nile fever also looks like the flu. About half of patients have a rash towards the end of the disease. Usually West Nile fever does not require treatment. This infectious disease is widespread in all countries of the world.

Culex pipiens mosquitoes are a vector for West Nile virus. Fabrizio Montarsi, CC BY 3.0, via Wikimedia Commons
West Nile virus can cause fatal neurological disease in humans.
However, around 80% of those infected remain asymptomatic.
West Nile virus is mainly transmitted by the bites of infected mosquitoes.
It can also cause serious illness and death in the horse.
There are vaccines for horses, but not yet for humans.
Birds are the natural hosts of West Nile virus.
West Nile virus (WNV) can cause neurological disease in humans and lead to death. It is commonly found in Africa, Europe, the Middle East, North America, and West Asia. It is maintained in nature through a cycle involving transmission between birds and mosquitoes. It can infect humans, horses and other mammals.
West Nile virus (WNV) belongs to the flavivirus genus and the Japanese encephalitis antigen complex, in the family Flaviviridae.
Human infection most often results from the bites of infected mosquitoes. These insects become infected by feeding on infected birds, in which the virus remains in the bloodstream for a few days. The virus ends up migrating into the mosquito’s salivary glands. In subsequent meals (when the insect stings), the virus can be injected into humans or animals. It then multiplies and can cause disease.
Either the WNV infection is asymptomatic, in about 80% of people, or it causes West Nile fever. It can also progress to serious illness.
About 20% of infected people develop West Nile fever. The clinical picture includes fever, headache, asthenia, pain, nausea, vomiting, and occasionally a rash (on the trunk) and lymphadenopathy (swelling of the glands).
West Nile virus can be diagnosed using a number of methods:
- Seroconversion of IgG antibodies (or significant increase in antibody titers) in two series of samples taken one week apart by enzyme-linked immunosorbent (ELISA);
- IGM by immunoenzymology (ELISA);
- Neutralization tests;
- Viral detection by RT-PCR (reverse transcription – gene amplification);
- Isolation of virus in culture.
IgM can be detected in virtually all cerebrospinal fluid (CSF) and serum samples received from WNV infected patients at the time of clinical presentation. Serum IgM can persist for more than a year.
For patients with a neuroinvasive form of West Nile virus infection, treatment is symptomatic and often requires hospitalization, intravenous infusions, respiratory support, and prevention of secondary infections. There is no vaccine for humans.
The risk of tropical diseases from contaminated water and food
Diarrhea is the most common disease contracted in the tropics. Although usually not very serious (tourista), it can sometimes be caused by parasites (filariasis…), bacteria (typhoid, shigellosis, salmonellosis) or viruses (hepatitis A), the symptoms of which are more serious.
Simple hygiene rules can prevent these infections. Thus, you should only drink bottled, boiled or disinfected water (beware of ice cubes made from tap water), eat only peeled or washed fruits and vegetables, well-cooked and hot meats, fresh fish…
In addition to these precautions, there are vaccinations against hepatitis A and typhoid, especially when traveling in poor hygienic conditions.
Tropical diseases transmitted by insects
Other diseases transmitted by mosquitoes are chikungunya and yellow fever (for which there is a lifelong vaccine available).
Other insects can transmit tropical diseases such as:
- Tse-Tse flies causing sleeping sickness (trypanosomiasis);
- sandflies giving leishmaniasis (oriental sore);
- the so-called triatomine bugs or reduva, which cause Chagas disease.
Tse-Tse flies
African trypanosomiasis or sleeping sickness is a parasitic disease of humans and other animals. It is caused by a parasite caused by the bite of the Tsetse fly with a parasite of the species Trypanosoma brucei which attacks the central nervous system and can lead to death. The tsetse fly is the main vector of sleeping sickness, otherwise known as Human African Trypanosomiasis (HAT).
Found in sub-Saharan Africa, it mainly affects rural populations who subsist on agriculture, fishing and livestock activities. Characterized by fever, joint pain and damage to the central nervous system, can be fatal if not treated. Currently there is no vaccine to prevent the disease. And “its development appears to be difficult because of the trypanosome’s ability to override the mammalian immune system”. “Disease screening and treatment [on the other hand] is expensive, painful and toxic. “Therefore, “vector control remains the only way to break the transmission cycle for now”.
Leishmaniasis (oriental sore)
Leishmaniasis comes in 3 main forms: visceral (the most severe, often called kala-azar), cutaneous (the most common) and mucocutaneous.
Leishmaniasis is caused by a protozoan of the genus Leishmania, transmitted by the bite of an infected sandfly.
The disease, which affects some of the world’s poorest populations, is associated with malnutrition, population displacement, unsanitary housing, a weakened immune system and lack of financial resources.
There is a link between leishmaniasis and certain environmental changes, such as deforestation, dam construction, irrigation systems and urbanization.
Infestation with Leishmania parasites only progresses to the disease stage in a small proportion of infected people.
The diagnosis of visceral leishmaniasis is made on the basis of a clinical examination combined with parasitological or serological tests (particularly rapid diagnostic tests). For the cutaneous and mucocutaneous forms of the disease, serological tests are of limited value and the diagnosis is based on observation of clinical manifestations and confirmation by parasitological tests.
There is currently no vaccine or prophylactic medication.
The treatment of leishmaniasis depends on several factors, including the form of the disease, concomitant conditions, the parasite species and the geographical location. Leishmaniasis is a disease that can be treated and cured, but requires a competent immune system because the drugs do not completely eliminate the parasite from the body, so there is a risk of relapse if immunosuppressed. Full treatment should be given promptly to all patients diagnosed with visceral leishmaniasis.
Chagas (disease, American trypanosomiasis)
It is estimated that six to seven million people are infected with Trypanosoma cruzi (T. cruzi), the parasite that causes Chagas disease, worldwide. Most of these people live in Latin America.
Chagas disease is a vector-borne disease that is transmitted to humans mainly in Latin America through an insect called a triatomine cell, which can carry T. cruzi.
Other modes of transmission of Chagas disease include: oral transmission (through food), transfusion of blood / blood products, mother-to-child transmission (congenital), organ transplantation and laboratory accidents.
Chagas disease previously affected only rural areas of the Region of the Americas, and especially Latin America. In recent decades, however, population movements have resulted in most of the infected people living in urban areas (urbanization) and the disease has spread to other continents (where T cruzi is transmitted via non vector).
T cruzi infection is curable if treated quickly.
In chronically infected people, antiparasitic treatment can potentially prevent or stop the progression of the disease, and prevent its transmission, including infection from mother to child.
Up to 30% of chronically infected people have heart problems, and up to 10% of them suffer from digestive and / or neurological problems, which may require special treatment.
The most effective methods of preventing Chagas disease in Latin America are vector control and other strategies to reduce vector transmission.
Globally, blood screening plays a crucial role in preventing infection through transfusion or organ transplantation.
It is essential to detect and treat the infection in women and girls of childbearing age, as well as to screen any newborn and siblings for screening in case the mother is infected and has not. never received antiparasitic treatment.
Certain socio-economic and environmental factors strongly influence Chagas disease, the spread and different interdependent dimensions of which justify the need to implement multisectoral control strategies.
People with Chagas disease are at risk of developing acute symptoms of COVID-19 and should be among the priority groups for vaccination.
To treat Chagas disease, hospitalization is necessary in a very specialized environment (tropical medicine department).
Chagas disease can be treated and the parasite eliminated with benznidazole or nifurtimox. If given soon after infection, from the onset of the acute phase, both drugs are almost 100% effective in treating disease, including cases of congenital transmission. The further back the infection, however, the more effectiveness of benznidazole and nifurtimox decreases. The two drugs also cause side effects more frequently in the elderly. However, they are also indicated for people in whom the infection has been reactivated (for example due to immunosuppression) and for patients who are entering the chronic phase of the disease. In particular, they may be prescribed to women and girls of childbearing age (before or after pregnancy) to prevent congenital transmission.
Treatment should be offered to infected adults, especially those without symptoms, as antiparasitic treatment can prevent or stop the progression of the disease. In other cases, it is necessary to weigh, on the one hand, the advantages of drug therapy in preventing or delaying the development of Chagas disease, and on the other hand, the duration of treatment (up to after two months) as well as possible side effects (observed in a percentage of adult patients sometimes up to 40%). Benznidazole and nifurtimox should not be given to pregnant women or to people with renal or hepatic impairment. Nifurtimox is also contraindicated in people with a history of neurological or psychiatric disorders. Finally, special treatment may need to be prescribed if heart, digestive or neurological disorders develop.
Tropical diseases: other risks
Freshwater swimming
In some tropical destinations, the risk of bilharzia (disease caused by a parasite living in fresh, stagnant water) and leptospirosis is still high.
Onchocerciasis, or “river blindness” is an infectious disease caused by parasitic worm larvae that crawl under the skin when swimming in fresh water.
This disease results in very strong itching, potentially disfiguring. The larvae can also enter the eye, causing visual impairment that can lead to blindness.
Barefoot walk
Strongyloidiasis or anguillulosis is an intestinal disease caused by a parasite present in contaminated soil. The infection is most often made on a beach, by skin contact with the sand.
Wild animals
The risk of rabies from bites by wild animals is more common in tropical countries. There is a rabies vaccine that extends the length of time you can receive treatment.
Bacterial infections in Tropical Disease
Meadow or Hansen’s Disease (Leprosy)
This is because, left untreated, leprosy is a decaying disease caused by a bacterium, Mycobacterium leprae. Transmission occurs between individuals via droplets from nasal and oral secretions (Flügge droplets), incubation can then range from 5 to 20 years. Symptoms are represented by damage to the skin, nerves, eyes leading to tissue atrophy. Treatment is based on multiple antibiotic therapy but the disease is curable on condition that the treatment is appropriate and early. The BCG vaccine has a certain preventive effect against leprosy.
Buruli ulcer
The prevalence of Buruli ulcer is unknown but this pathology is found in Africa, Asia, and Latin America.
The disease is caused by a bacterium, Mycobacterium ulcerans, causing cutaneous lesions of the type of nodules then ulcers which can become superinfect and causing deformities responsible for handicaps. The risk of mortality is low, although secondary infections of the initial lesions can be fatal. Treatment is surgery and antibiotics, and when it is early, it helps prevent most symptoms from developing.
Trachoma
It is found in Africa, Asia, Central and South America, the Middle East and Australia. The disease preferentially affects women and children. Despite a poor functional prognosis, the risk of mortality is very low.
The disease is caused by a bacterium, Chlamydia trachomatis, which spreads from eye secretions on hands, clothes or even flies drinking from these secretions. The symptoms consist of inflammation of the inner surface of the eyelids causing a deformation of the structure of the eyelid and contact of the eyelashes with the cornea which becomes cloudy by friction. The treatment uses antibiotics, the first of which is azithromycin in eye drops. The only known prevention is personal hygiene. Repeated treatment and education campaigns for the populations concerned seem to have had very little effect, while the only effective preventive measure remains access to basic education for the populations affected.
Yaws
There are few data on the prevalence of yaws, but we know that it preferentially affects children. The disease is most prevalent in hot and humid regions of Africa, Asia, South America and the islands of the Pacific Ocean.
It is a chronic bacterial disease transmitted by contact and caused by a treponema, Treponema pallidum pertenue. Treatment is based on antibiotics (especially penicillin) and the disease can be prevented by simple personal hygiene measures. The symptomatology is represented by ulcerated skin lesions on a budding background which can most often become superinfect and possibly abscess. Although the risk of mortality is low, the functional prognosis may be poor due to disabling lesions, in addition to a major aesthetic prognosis, especially in the event of a facial lesion.
Verminosis
Cysticercosis and taeniasis
Cysticercosis and more generally taeniasis are parasitic diseases caused by tapeworms. Indeed, it is the larva of Taenia solium which is responsible for cysticercosis while the adult worm of many species such as Taenia solium or Taenia saginata for the best known, but also Hymenolepis nana, Dipylidium caninum or Diphyllobothrium latum is responsible for taeniasis. These diseases are helminthiasis. Cysticercosis is the leading preventable cause of epilepsy in developing countries. Although cosmopolitan, these pathologies are found mainly in Asia, sub-Saharan Africa and Latin America.
Unlike cysticercosis, which in its neurological form can be fatal, tæniasis does not result in the death of the patient. These infections are contracted orally by ingesting Taenia solium eggs during a meal contaminated with human stool for cysticercosis, or by eating contaminated pork, beef or fish. for tæniasis. The symptomatology of tæniasis is usually quite crude, including abdominal pain, nausea, constipation, diarrhea, sleep disturbances or irritability. Cysticercosis, on the other hand, due to its neuromeningeal tropism involves the formation of cysts and cerebral lesions which can be the cause of headache, blindness, critical episodes, hydrocephalus, meningitis or even dementia30. Anthelmintic drugs such as albendazole or flubendazole are commonly used to treat these conditions. A cysticercosis cerebral localization makes consider concomitant immunosuppressive treatment with corticosteroids. Prevention mainly involves hygiene measures including examination of the meat before consumption, thorough cooking in order to kill eggs or larvae, limitation of the spreading of human excreta for the purpose of soil fertilization or even the spreading of human excreta. ” access to an efficient sewerage system.
Echinococcosis
Two distinct diseases caused by two different parasites are grouped together under the term echinococcosis mainly: alveolar echinococcosis (Echinococcus multilocularis) and cystic or hydatid echinococcosis or hydatidosis (Echinococcus granulosus). Cystic echinococcosis is found in the eastern Mediterranean, in North Africa, in the southern half of South America, in Central America in Central Asia. Alveolar echinococcosis is found in western and northern China, Russia, Europe and North America.
The disease is caused by the ingestion of parasites found in the stools of certain wild animals, typically canines. Both infections involve an incubation period of several years. Cystic echinoccocosis causes, as the name suggests, liver cysts called hydatid cysts causing abdominal pain, nausea and vomiting. These cysts can also be found in the lungs, causing coughing, chest pain and dyspnea. Alveolar echinococcosis also begins with a cyst, usually hepatic, which will gradually invade the organ, causing asthenia, abdominal pain, nausea and vomiting and which may, after a course of several years, induce hepatic insufficiency, cirrhosis of the liver or liver cancer. Thus, untreated echinococcosis can be fatal. The disease is diagnosed by medical imaging techniques and serological tests. The treatment of echinoccocosis is both surgical and drug concomitant with surgery by administration of albendazole. The disease could have been prevented by deworming pets, improving the conditions for eliminating their stools, improving overall hygiene conditions, particularly with regard to food and drink.
Dracunculiasis
Dracunculiasis is also known as Filariasis of Medina. In 2012, the four endemic countries were Chad, Ethiopia, Mali and South Sudan.
The disease is caused by a helminth, Dracunculus medinensis, also called Medina wireworm or Guinea worm. Transmission occurs through ingestion of water infested by aquatic crustaceans, cladocerans, themselves infected by the larva of Dracunculus medinensis36. The pathology is not lethal in itself, but can be the cause of prolonged inactivity due to the lasting and disabling wounds it induces. The treatment consists of cleaning and bandaging the wounds caused by the outcome of the parasite about a year after infection, generally in the distal zone of the lower limb (classically, the perimalleolar zone). This is associated with the very slow extraction of the parasite by surrounding it around a small piece of wood. The extraction is of the order of a centimeter per day, the treatment thus being very long, the parasite being able to measure more than one meter in length. A faster extraction is dangerous because of the risk of rupture of the parasite which would lead to significant allergic disorders in the patient which could lead to anaphylactic shock and then death. Dracunculiasis can be prevented by filtering water, quickly identifying cases to prevent the risk of spread, and treating drinking water with larvicides. As the parasite’s cycle is long, of the order of a year, these methods are quickly effective when followed on a population scale.
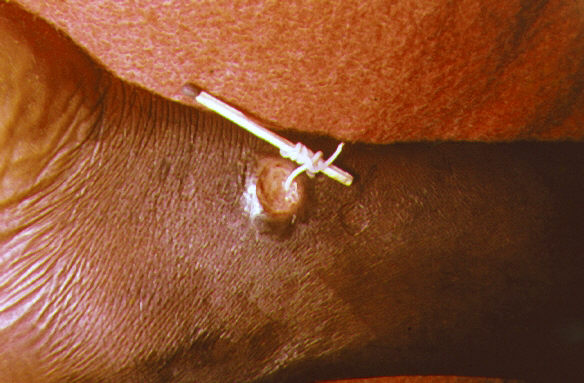
Dracunculus medinensis. Dracunculosis/Guinea Worm Disease. A method used to extract a Guinea worm from the leg vein of a human patient. CDC, Public domain, via Wikimedia Commons
Lymphatic filariasis
Lymphatic filariasis, causing the impressive elephantiasis, affects approximately 120 million people of which 40 million are affected by deformities. These cases are distributed for two thirds in South-East Asia, the remaining third being found in sub-Saharan Africa.
The disease can be caused by different nematode species: Wuchereria bancrofti (Bancroft filaria, the most common), Brugia malayi (Malayan filariasis) and Brugia timori. It is a vector-borne disease transmitted by various species of mosquitoes of the genera Anopheles, Culex, Aedes or Mansonia. The disease is rarely fatal, but the damage from the parasite lasts for the rest of a patient’s life. They consist of lymphoedemas of the limbs, genital pathologies and painful crises. Most infected patients are asymptomatic but have damage to the lymphatic system, and more than 40% of infected patients have kidney damage that can lead to kidney failure. The diagnosis is made by the parasitological examination of the patient’s blood, taken in the middle of the day or in the middle of the night (generally both) depending on the infecting species considered. The historical treatment of filariasis is diethylcarbamazine. However, an anthelmintic treatment based on ivermectin or albendazole or even praziquantel is effective. Another strategy consists of the administration of doxycycline, an antibiotic targeting Wolbachia, the parasite’s symbiotic bacteria. Prevention involves controlling the vectors and their bites and the preventive administration of filaricides and microfilaricides.
Onchocerciasis
Onchocerciasis, also known as “river blindness”, affects an estimated 37 million people 9, 99% in sub-Saharan Africa, especially in rural areas. The disease is caused by a heartworm, Onchocerca volvulus, transmitted by a blood-sucking fly of the genus Simulia. These are the characters of the vector that explain the classic name of “river blindness”, the black flies are mainly found along moving, shady and aerated streams. Thus, onchocerciasis causes the displacement of populations away from freshwater points and the abandonment of entire villages.
The parasite in the larval stage causes blindness, skin rashes, depigmentation of the skin and itching. The disease can be treated with ivermectin and prevented by the application of insecticides and the administration of anthelmintics as a preventive measure.

Cameroonian with Onchocerciasis. Mectizan Donation Program, CC BY-SA 4.0, via Wikimedia Commons
Bilharzia
There are over 200 million cases of bilharzia10 (also called schistosomiasis) worldwide. It is estimated that 85% of these cases are located in sub-Saharan Africa10, the vast majority of which are intestinal and urinary bilharziasis, although there are particular clinical forms due to certain specific species in other regions of the world, particularly in South Asia.
The different species of Schistosoma have a complex parasitic cycle where humans are the definitive host while freshwater mollusks act as the intermediate host, each species of schistosome having a different mollusc as an intermediate host. Infection occurs upon skin contact with contaminated water. The organ damage resulting from infection is not so much due to the worm itself or its larva, but to the large number of eggs produced by the parasites. The classic consequences are represented by hematuria, bladder obstruction, renal failure, bladder cancer, periportal fibrosis then consequently portal hypertension, ascites, upper digestive hemorrhages following the onset. esophageal varices 9. Thus, the disease can be fatal after a relatively long course. Infection with the parasite also causes cervical lesions in women and young girls, increasing the risk of HIV transmission.
The disease can be diagnosed by serological testing, which produces many false positives, but also by direct examination of stool and urine (possibly sputum) for eggs. Praziquantel is used to treat patients with schistosomiasis but does not prevent re-infection. The cost of prevention is estimated at US $ 0.32 per child per year and would consist of mass administration of praziquantel, better access to clean water, improved hygiene conditions and health education for children. populations concerned. Vaccines are also under development, including Bilhvax.
Digestive nematodoses
The term digestive nematodosis includes, in the context of neglected tropical diseases, trichocephalosis (Trichuris trichiura), ascariasis (Ascaris lumbricoïdes) and hookworm infection (Ancylostoma duodenale and Necator americanus). An estimated 1.5 billion people are infected with these organisms. Gastrointestinal nematodoses are found in sub-Saharan Africa, Central and South America, China and Southeast Asia.
Transmission of these parasitic worms is usually due to exposure to infected stool through the skin or intestines (faecal hazard), spread through practices such as open defecation or the application of human stool as agricultural fertilizer. The most common symptoms are anemia, stunted growth, reduced physical ability, as well as academic performance and attention. The severity of the disease depends largely on the parasite load of the patient, but can include intestinal problems and asthenia that can compromise the physical and cognitive development of affected children45. Drug treatment with flubendazole, albendazole or ivermectin can often be sufficient, but the use of digestive surgery is sometimes necessary in cases of very high parasite load or digestive complications. These diseases can be prevented by improving domestic hygiene conditions and wastewater treatment infrastructure, access to clean water and clean food preparation measures. WHO recommends deworming without prior diagnosis in the most affected regions of the world.

Ascaris Lumbricoides that had caused intestinal obstruction. Nmitei, CC BY-SA 4.0, via Wikimedia Commons
Virus of Tropical Diseases
Dengue
The number of symptomatic infections with the dengue virus is estimated to be between 50 and 100 million annually46. Dengue cases are found mainly in Asia, Latin America and northern Australia46.
Dengue fever is an arbovirus caused by a flavivirus transmitted by the bite of a mosquito, Aedes aegypti, during its blood meal46. There is no treatment other than symptomatic46. The symptoms are not very specific, associating fever, headache, arthralgia, myalgia, thus mimicking a flu syndrome46. Dengue is not lethal in the majority of cases, but infection with one of the four serotypes can increase the severity of subsequent infection with another serotype, resulting in severe and potentially fatal dengue.
Rabies
The prevalence is higher in rural areas and primarily affects children in Asia and Africa.
Rabies is usually fatal after symptoms develop. The disease is caused by a Rhabdoviridae of the genus Lyssavirus transmitted through wounds or bites by infected animals. There are two forms of rabies: furious and paralytic. It is estimated that 60,000 people die of rabies each year. The first symptoms are fever and pain at the site of infection between 1 and 3 months after the incubation period. Furious rabies, the most common type of rabies, causes hyperactivity (excitable), hydrophobia and aerophobia before death occurs from cardio-respiratory arrest within days. Paralytic rabies slowly progresses to generalized paralysis, then coma and finally death. Rabies cannot be diagnosed before symptoms start but can be detected after symptoms start. It can be prevented by vaccinating humans and non-human animals such as dogs by cleaning and disinfecting wounds (post-exposure prophylaxis), but there is no cure.
Zika virus
A Zika virus infection is accompanied by symptoms similar to those of the average flu and does not usually cause complications. The disease is most prevalent in Central and South America as well as Southeast Asia. The disease is dangerous, when a pregnant woman contracts the virus. Because the Zika virus can cause permanent microcephaly for the unborn child.
Yellow fever
Yellow fever is manifested by fever, headache and nausea during the first phase of the disease. About 15% of patients go through a second phase of the disease. This can cause damage to internal organs and the nervous system. Yellow fever is present in South America and Central America as well as in tropical countries in Africa.
Other neglected tropical diseases
Snake bite
The WHO lists snakebites as “another neglected condition”. Snakebites are a public health problem in rural areas of Africa and South and Southeast Asia. However, there is no official WHO program for the diagnosis, treatment or prevention of snakebites.
Sources: PinterPandai, World Health Organization (WHO), Centers for Disease Control and Prevention (CDC), American Society of Tropical Medicine and Hygiene, Frontiers
Photo credit: Edvard Munch (1863–1944) / Wikimedia Commons
Photo explanation: The Sick Child I by Edvard Munch, 1896, lithograph, Bergen Kunstmuseum.



