Acute Liver Failure
Acute hepatic failure or liver failure is defined as a major and overall impairment of liver function occurring over a period of a few days to a few weeks (with a previously normal liver). The severity of hepatitis is defined by the assessment of the overall function of the liver represented by the level of prothrombin (PT): we speak of severe acute hepatitis when the PT is less than 50%. When the patient additionally shows signs of neurological damage (called hepatic encephalopathy and a whole range of disorders up to coma), it is called fulminant hepatitis.
Liver failure, also known as acute liver failure, is a severe and life-threatening condition where the liver suddenly loses its ability to function properly. It is a medical emergency that requires immediate attention and intervention. Below, we outline the causes, symptoms, diagnosis, and treatment of acute liver failure:
Causes of liver failure
Why and how is it developing?
The main causes of severe hepatitis are viral infection (mainly hepatitis E, hepatitis A and hepatitis B viruses) and the voluntary or involuntary taking of medicines (including paracetamol first) or drugs. The other causes mainly encountered are an immunological disorder, an inherited disease (such as an accumulation of copper in the body), and poor vascularization of the liver (dysfunction of the heart, blood clot in a vessel draining the liver). Sometimes no cause is found.
What are the causes ?
There are two causes of liver failure:
A cirrhosis in terminal evolution: “it is the form of evolution of all the chronic diseases of the liver. Whether it is linked to the hepatitis B virus, hepatitis C, to alcohol or to other causes autoimmune, when we cannot prevent the progression of the disease, cirrhosis occurs, gradually leading to the destruction of liver cells and liver failure which can lead to the death of the patient if he cannot be transplanted”.
Acute hepatitis which may be linked to toxic hepatitis B such as paracetamol poisoning, or drug allergy. “For paracetamol there is an antidote if it is given early enough”, adds the gastroenterologist.
Causes:
- Viral Hepatitis: Infections caused by hepatitis A, B, C, D, and E viruses can lead to acute liver failure.
- Drug-Induced Liver Injury: Overdosing on medications or exposure to toxic substances can cause liver damage.
- Autoimmune Hepatitis: The body’s immune system mistakenly attacks the liver, leading to inflammation and damage.
- Wilson’s Disease: A genetic disorder that causes copper to accumulate in the liver, leading to liver damage.
- Acetaminophen (Paracetamol) Overdose: Taking excessive amounts of acetaminophen can result in liver toxicity.
- Budd-Chiari Syndrome: Blood clots block the veins that drain the liver, causing liver failure.
- Ischemic Hepatitis: Reduced blood flow to the liver due to heart failure or shock can lead to liver damage.
Read also: Hepatitis Viruses (A to G) | Transmission, Symptoms and Prognosis, Prevention
What are its main symptoms?
The clinical signs are quite rough at first and are often not noticed by the patient until the hepatitis has become severe or fulminant. They include fatigue, jaundice (or jaundice, due to the accumulation under the skin of bilirubin not metabolized by the liver), digestive disorders, an increase in abdominal volume (due to the appearance of water, called ascites, in the peritoneal cavity and secondary to liver dysfunction) and / or minimal bleeding (due to poor blood coagulation secondary to liver dysfunction). Neurological disorders can range from a simple ideomotor slowdown, to abnormal muscle movements, to coma. They are secondary to a defect in the purification of toxins by the liver, with an accumulation of these toxins in the brain.
The liver has an important role in the functioning of the body, and severe acute hepatitis or the decompensation of severe cirrhosis can lead to dysfunction of several organs. The brain can thus be affected as seen above. The heart and kidneys can also be affected with low blood pressure and kidney dysfunction that may require dialysis. Often patients require mechanical assistance to breathe, both for neurological disorders and for lung damage. On the other hand, severe acute hepatitis predisposes to infections.
Symptoms:
- Jaundice (yellowing of the skin and eyes)
- Abdominal pain and swelling
- Nausea and vomiting
- Fatigue and weakness
- Mental confusion and disorientation
- Easy bruising and bleeding
- Changes in behavior and personality
- Coma or loss of consciousness in severe cases.
How can I be diagnosed with it?
In the event of advanced chronic liver disease, called cirrhosis, the functioning of the liver can remain normal for several years and then suddenly be altered, this is called decompensation of cirrhosis. Again, hepatic failure is assessed by prothrombin levels and neurological signs. However, in cirrhosis, other parameters, such as the presence of fluid in the abdominal cavity, called ascites, the blood level of bilirubin, a protein that reflects the proper functioning of the liver, as well as that of albumin, a protein synthesized by the liver, are added to combine in a severity score called the Child-Pugh score. In very severe liver damage, when it is thought that only a liver transplant would cure, another score called the MELD score is used, combining the bilirubin level, the prothrombin level, the creatinine level. which reflects the functioning state of the kidneys. This score is used when registering for the transplant list, and a higher score allows faster access to the transplant.
Diagnosis:
- Physical examination to assess symptoms and signs of liver failure.
- Blood tests to measure liver function, clotting factors, and assess for signs of infection.
- Imaging tests like ultrasound, CT scan, or MRI to evaluate liver size and detect abnormalities.
- Liver biopsy, in some cases, to examine liver tissue for diagnosis and treatment planning.
Treatment and prevention of acute liver failure
The treatment of severe hepatitis is based on treating the cause (antiviral agent, antidote, for example) when it is available and on managing each organ dysfunction. When the acute hepatitis is fulminant with an unfavorable course despite maximal management, or when the cirrhosis is severe with a high Child-Pugh score and / or a high MELD score, it is necessary to react quickly to transfer the patient to an expert center in order to establish the indication for liver transplantation, in the absence of any contraindication.
Treatment:
- Hospitalization in the intensive care unit for close monitoring and support.
- Management of underlying causes such as viral infections or drug toxicity.
- Medications to stabilize liver function and manage complications.
- In some cases, liver transplantation may be necessary if the liver damage is irreversible.
Prevention:
- Vaccination against hepatitis viruses (A and B) can help prevent infections that lead to liver failure.
- Avoiding excessive alcohol consumption and being cautious with medications to prevent drug-induced liver injury.
- Seeking immediate medical attention if experiencing symptoms of acute liver failure.
Glossary
1. Prothrombin
Protein made by the liver which is transformed into thrombin and triggers blood clotting. This protein is used to measure liver failure with factor V. Vitamin K deficiency also causes a drop in prothrombin levels (PT expressed in%), unlike factor V which is not affected by the deficiency. in vitamin K or a treatment not anti-vitamin K.
2. Bilirubin
Bile pigment, the main product of the breakdown of red blood cells, constituting bile, present in the stool and urine in conjugated form with glucuronic acid. The unconjugated form is called free (or indirect) bilirubin. After passing through the liver, it is glucuronidated and then eliminated by the bile ducts. The conjugated (or direct) form is the soluble form of bilirubin in biological fluids. An increase in plasma bilirubin above 50 μmol / L is accompanied by the development of jaundice.
3. Ascites
(Greek askos: besides swelling) liquid present abnormally in the peritoneal cavity (belly), the origin of which may be hepatic (portal hypertension, cirrhosis), cardiac, renal, cancerous (carcinosis), inflammatory or even infectious (tuberculosis) ).
Determining the origin of this effusion is primarily based on the analysis of the fluid after a puncture (ascites puncture).
4. Albumin
(Comes from Latin albumen: egg white) blood protein produced by the liver. It participates in the transport in the blood of certain hormones and drugs and provides 70% of the oncotic pressure of plasma and. Albumin levels are used to measure the degree of liver failure in cirrhosis.
Sources: PinterPandai, WebMD, Mayo Clinic, Massachusetts Medical Society, National Center for Biotechnology Information (NCBI)
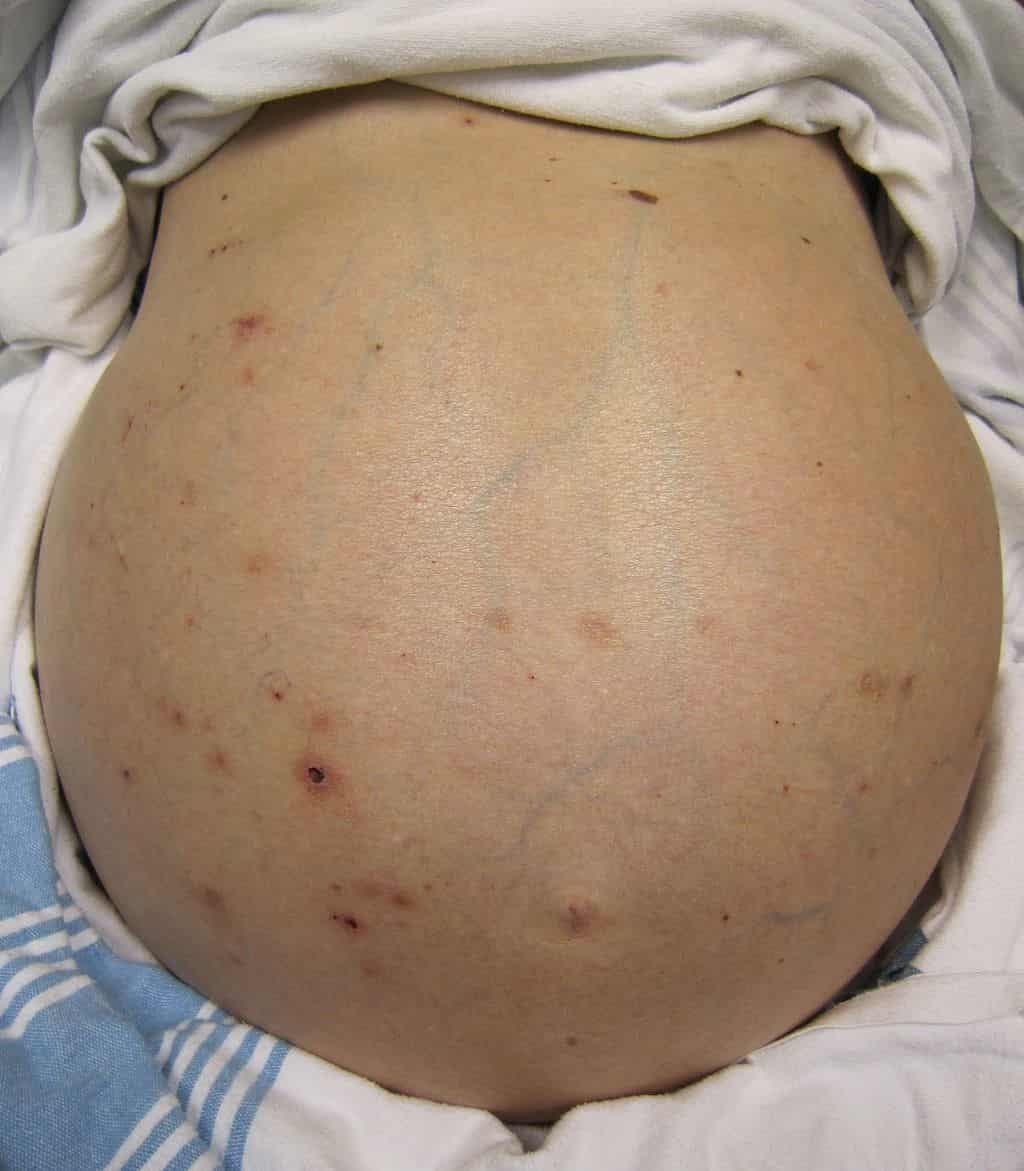
Photo credit: James Heilman, MD / Wikimedia Commons
Photo explanation: a person with massive ascites caused by portal hypertension due to cirrhosis.