Lupus Disease
Lupus disease is an autoimmune disease where the immune system attacks healthy cells, affecting various body parts like joints, skin, kidneys, and heart.
What are the first signs?
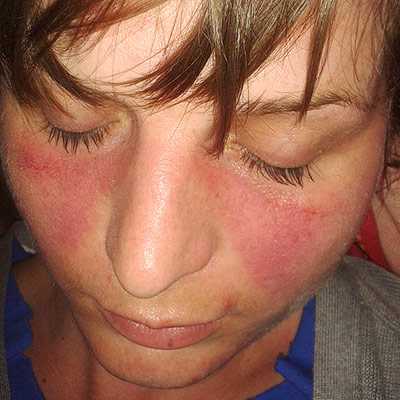
The wolf-shaped facial rash characteristic of lupus. The most suggestive symptom of systemic lupus erythematosus is a rash on the face, appearing during a flare-up of the disease. These red plaques predominate on areas of skin exposed to the sun (photosensitivity).
What are the pains of lupus?
Joint pain and inflammation (arthritis) are very common. They mainly affect the fingers, hands, shoulders and knees. But unlike rheumatoid arthritis (RA), lupus rarely destroys the joints.
Causes & Network
The immune system is a complex network of organs, tissues, and cells. For reasons we still don’t know (perhaps environmental, hormonal and genetic factors), the body makes antibodies that attack its own healthy tissue.
Disease Evolution
Lupus is characterized by alternating flare-ups and periods of remission. Flare-ups involve abnormal antibodies attacking the body, while remission can last for weeks, months, or years.
Definition and Explanations
This disease occurs when the immune system attacks cells in the body and destroys them. It can affect many parts of the body, including joints, skin, kidneys, heart, etc. This is why it is called systemic or “systemic” lupus. Lupus can cause symptoms as different as unexplained fevers, joint pain and swelling, blurred vision and many more. It mainly affects women of childbearing age, from 15 to 40 years old. The symptoms and severity vary widely from person to person.
Lupus Triggers
Stress, overwork, sun exposure, and becoming pregnant or giving birth can trigger this disease by a mechanism that is not yet known. Also, certain medications used to treat another illness can trigger symptoms of this disease. This is called drug lupus. Symptoms usually go away when the person stops taking the offending drug. Researchers believe that exposure to certain substances, such as pesticides, mercury or silica, also increases the risk.
[Image of the lupus butterfly rash diagram]
What are the types of lupus?
Formerly “systemic lupus erythematosus,” it affects many parts of the body. A person might experience joint pain, skin rashes, and kidney issues simultaneously.
Limited to the skin. Manifests as well-limited, symmetrical patches on the face or scalp. It can leave unsightly permanent scars, making urgent treatment necessary.
Exclusively affects the skin on the face. Treatments like UV protection and antimalarials help improve appearance and prevent new lesions.
Triggered by medications like doxycycline, Bactrim®, or beta-blockers. Symptoms usually go away when the medication is stopped.
Linked to anti-SSA or SSB antibodies in the mother affecting the fetus. A baby may have a rash or liver issues, which usually resolve over time.
Forms limited strictly to skin rashes and sun sensitivity without internal organ involvement.
Lupus Symptoms Detail
Non-Specific Symptoms
- Extreme tiredness
- Unexplained weight loss or gain (fluid retention)
- Unexplained bouts of fever
- Swollen glands
Specific Symptoms
- Pain, stiffness, and swelling in joints (arthralgia)
- Butterfly-shaped red patch on cheeks/nose
- Extreme sun sensitivity (red rashes)
- Crusty, disc-shaped patches on face/scalp
- Painless sores (ulcers) in mouth or nostrils
- Chest pain during deep breaths (lung damage)
- Swelling of the legs (oedema)
- Arrhythmia or heart failure
Other Symptoms
Hair loss, blurred vision, dry eyes, Raynaud’s disease (blue fingers/toes in cold), hives, headaches, seizures, blood clots (thrombosis), and kidney damage (detected by urine tests). Includes susceptibility to infections and Anemia.
Treatments and Medication
Drug treatments
Immunoglobulin infusions: Obtained from donor blood. They neutralize auto-antibodies and are reserved for cases resistant to other treatments like corticosteroids.
Pain medications: Acetaminophen (Tylenol®) and NSAIDs (ibuprofen) ease joint pain. However, severe lupus patients should avoid over-the-counter painkillers as they increase kidney damage risk.
Corticosteroids (Prednisone): Used since the 1960s to reduce inflammation. Long-term use side effects include bruising, mood swings, diabetes, cataracts, high blood pressure, and osteoporosis.
Anti-malarial drugs: Hydroxychloroquine (Plaquenil®) and chloroquine (Aralen®) treat joint pain, swelling, and skin rashes. They are also used to prevent sun damage and relapses.
Immunosuppressants: Used when prednisone fails or for kidney/nervous system involvement. Examples include cyclophosphamide (Cytoxan®), azathioprine (Imuran®), mycophenolate mofetil (Cellcept®), and belimumab (Benlysta).
Final Summary & Life Expectancy
The survival prognosis has improved dramatically. Life expectancy exceeds 95% at 10 years with appropriate care. Treatment focuses on managing symptoms and minimizing flare-ups through medication and lifestyle adjustments.
Information: Cleverly Smart is not a substitute for a doctor. Always consult a doctor for your health condition.