Leukemia
Leukemia is cancer that starts in blood stem cells. Stem cells are basic cells that turn into different types of cells that have different functions.
Types of Leukemia
There are many different types of leukemia. They are first classified according to the type of blood stem cell from which they develop. Lymphoid leukemia (also called lymphoblastic leukemia) starts in abnormal lymphoid stem cells. Myeloid leukemia (also called myelogenous leukemia) is caused by abnormal myeloid stem cells.
The types of leukemia are then further subdivided based on how quickly the disease grows and progresses. Acute leukemia starts suddenly and develops over a few days or weeks. Chronic leukemia develops slowly over months or even years.
The 4 main types of leukemia are Acute Lymphoblastic Leukemia (ALL), Acute Myelogenous Leukemia (AML), Chronic Lymphoid Leukemia (CLL) and Chronic Myeloid Leukemia (CML).
In adults, the most common leukemias are CLL and AML. There are many different subtypes of leukemia.
Types
There are several forms of leukemia, depending on the degree of maturity of the abnormal cells, and molecular abnormalities.
• Acute Lymphoblastic (ALL)
It progresses very quickly, and its complications can be dangerous very quickly. It is a medical emergency, requiring the patient to be hospitalized quickly.
It characterized by the proliferation of lymphocytes which places it in the category of chronic lymphoid hemopathies. It is the most common leukemia, affecting people over 50 years of age. Apart from a few familial cases, we do not know of any factors favoring the onset of the disease, be they environmental, genetic or infectious. This affection is incurable to this day, but the prognosis is extremely variable from one patient to another. For 60% of patients it is not necessary to start treatment at the time of the initial diagnosis of the disease given its slow progress.
• Chronic (CLL)
There are other forms of leukemia, such as chronic leukemia, which are seen in adults only. In this case, the malignant cells are generally well differentiated and the symptoms appear late, in a quieter manner.
• Myeloid (AML)
Leukemia is called myeloid (or myeloblastic) or lymphoid (lymphoblastic) depending on the level of differentiation blockage of the leukemic cell. These are two very different types of leukemia. In children, the majority of leukemias are lymphoblastic, while in adults, leukemias are mainly myeloblastic.
• Chronic Myeloid (CML)
A monoclonal myeloid proliferation without blocking of maturation predominant on the granular line at the medullary and splenic level.
In humans, it is one of the 4 major myeloproliferative syndromes (with polycythemia vera, essential thrombocythemia and myeloid splenomegaly). It mainly affects adults between 30 and 50 years old and is favored by exposure to benzene and ionizing rays.
Symptoms of leukemia
The signs or symptoms of leukemia can vary depending on what form of leukemia you have, either acute or chronic.
Acute leukemia can cause flu-like signs and symptoms. They appear suddenly within days or weeks.
Chronic leukemia often causes few or no symptoms at all. Usually, signs and symptoms appear gradually. Many people with chronic leukemia just say they don’t feel well. The disease is often discovered during a routine blood test.
Other medical conditions can cause the same symptoms as leukemia. See your doctor if you experience these symptoms:
- tired
- general feeling of discomfort or illness (malaise)
- loss of appetite
- weightloss
- fever
- shortness of breath
- pallor
- fast heartbeat (palpitations)
- weakness
- dizziness
- bruising tendency
- frequent or heavy nosebleeds
- bleeding gums
- bleeding in the middle of the menstrual cycle or heavy periods
- small, reddish, flat spots on the skin caused by bleeding under the skin (petechiae)
- frequent infections of the lungs, urinary tract, or gums or around the anus
- frequent cold sores
- vomiting
- headache
- sore throat
- night sweats
- bone or joint pain
- swollen lymph nodes in the neck, armpits, groin or above the collarbones
- abdominal discomfort or feeling of fullness
- visual disturbances
- lesions in the eyes
- swelling of the testicles
- chloroma – clumps of leukemia cells, or blasts, under the skin or in other parts of the body
- skin leukemia – lesions or plaques of any size and usually pink or reddish-brown
- allergic angiitis – a disorder similar to an allergic skin reaction that usually manifests as sores on the hands and feet
Sweet’s syndrome, or acute febrile neutrophilic dermatosis – a condition characterized by fever and painful lesions that can occur anywhere on the body
Emergencies due to cancer
In some cases, leukemia or its treatments can cause serious problems. These cancer emergencies should be treated immediately.
Tumor lysis syndrome can develop when chemotherapy is given to treat acute leukemia and the cancer cells die quickly, not allowing the kidneys to remove the substances they release from the blood quickly enough. Find out more about tumor lysis syndrome.
Superior vena cava compression syndrome (SCVCS) can occur when too many leukemia cells form in the thymus, causing it to grow larger and block the trachea. SCVCS can occur in the presence of acute lymphoblastic leukemia (ALL). Find out more about superior vena cava compression syndrome.
Disseminated intravascular coagulation (DIC) is a disorder characterized by the formation of blood clots in the circulating blood and by bleeding. DIC occurs more often in the presence of acute promyelocytic leukemia, but it can also occur with other subtypes of acute myelogenous leukemia (AML). Find out more about disseminated intravascular coagulation.
Diagnosis of leukemia
It usually begins with a visit to your family doctor or when the results of a routine test suggest a blood disorder. Your doctor will ask you about your symptoms and may do a physical exam. Based on this information, your doctor may refer you to a specialist or order tests to check for leukemia or other health problems.
The process can seem long and overwhelming. It’s normal to worry, but try to remember that other medical conditions can cause leukemia-like symptoms. It is important that the healthcare team rule out any other possible cause of the condition before making a diagnosis of this cancer.
When symptoms are severe, the diagnostic process for acute leukemia can be done quickly, with the person being admitted to the hospital for prompt treatment.
The following tests are commonly used to rule out or diagnose leukemia. Many tests that can diagnose cancer are also used to determine its stage, that is, how far the disease has progressed. Your doctor may also give you other tests to check your general health and help plan your treatment.
| Diagnostic tests | Staging and other tests |
|---|---|
|
|
Health history and physical exam
Your health history is a record of your symptoms, risk factors and all the medical events and problems you have had in the past. In taking a health history, your doctor will ask questions about a personal history of:
- symptoms that suggest leukemia
- exposure to high doses of radiation
- genetic syndromes, such as Down syndrome, Fanconi anemia, ataxia-telangiectasia or Bloom syndrome
- exposure to benzene
- previous chemotherapy or radiation therapy
- blood disorders
- viral infections
Your doctor may also ask about a family history of leukemia.
A physical exam allows your doctor to look for any signs of leukemia. During a physical exam, your doctor may:
- check your vital signs to see if you have a fever, shortness of breath and rapid heartbeat
- check your skin for bruising and paleness
- feel areas of the neck, underarm (axillary) and groin (inguinal) for any swollen, or enlarged, lymph nodes
- check your mouth for infection, bleeding or swollen gums
- feel your abdomen for enlarged organs
- examine your skeleton for tenderness or pain
Complete blood count (CBC)
A CBC measures the number and quality of white blood cells, red blood cells and platelets. Leukemia and other conditions can cause abnormal blood cell counts.
Immature blood cells (called leukemia cells, or blasts) are not normally seen in the blood, so doctors will suspect leukemia if there are blasts or blood cells do not look normal.
Blood chemistry tests
Blood chemistry tests measure certain chemicals in the blood. They show how well certain organs are functioning and can help find abnormalities. They help doctors find problems with the liver or kidney that are caused by the spread of leukemia cells. They can also help doctors stage leukemia.
Levels of the following chemicals may be higher than normal with leukemia:
- blood urea nitrogen (BUN)
- creatinine
- phosphate
- lactate dehydrogenase (LDH)
- alanine aminotransferase (ALT)
- aspartate aminotransferase (AST)
- uric acid
Bleeding and clotting factors
Tests measure blood clotting factors to see how well the body can clot blood. Abnormal levels of blood clotting factors may occur with leukemia. They are measured using the following tests:
- fibrinogen level
- prothrombin time (PT)
- international normalized ratio (INR)
- partial thromboplastin time (PTT)
Cytochemistry
Cytochemistry uses stains, or dyes, to identify tissue structures and components in blood or bone marrow cells. Certain stains are attracted to certain substances found in some types of leukemia cells, or blasts. The staining results can be seen under a microscope. Cytochemistry helps doctors determine the type of cells that are present.
Immunophenotyping
Immunophenotyping is the study of proteins expressed by cells. It is used to determine the type or subtype of leukemia.
Immunophenotyping uses a very specific antigen-antibody reaction to identify proteins in tissues or cells. It uses monoclonal antibodies marked with a fluorescent label or specific enzyme label that binds only to specific antigens (proteins). The fluorescent or enzyme label allows doctors to see the leukemia cells (also called blasts).
Immunohistochemistry and flow cytometry are the 2 most common methods used in immunophenotyping for leukemia.
Immunohistochemistry
Immunohistochemistry uses a microscope to view the immunoperoxidase labels. It also allows doctors to look at cells and what is around them.
Flow cytometry
Flow cytometry is a technique used to sort and classify cells using fluorescent labels on their surface. The cells are exposed to a laser, which makes them give off a light. The light is measured and analyzed by a computer. Flow cytometry allows doctors to view many antibodies at the same time and collect data rapidly from thousands of cells in a single sample.
Flow cytometry helps to define unique features of leukemia cells, or blasts. These features can help doctors form a prognosis and measure response to treatment using minimal residual disease (MRD). MRD means that there are blasts in the bone marrow that can’t be found using standard lab tests (such as microscopy), but are found using more sensitive tests (such as flow cytometry or polymerase chain reaction).
Cytogenetic and molecular studies
Cytogenetics is the analysis of a cell’s chromosomes, including the number, size, shape and how they are arranged.
Cytogenetic karyotyping studies show chromosomal abnormalities, which help doctors confirm that someone has leukemia and find out the type or subtype of leukemia. The results of cytogenetic studies also help doctors plan treatment and predict how well the treatment will work.
Some major chromosomal abnormalities can be found by looking at cells under a microscope. But most changes in DNA need a closer analysis with other molecular studies, including fluorescence in situ hybridization (FISH) and polymerase chain reaction (PCR).
Fluorescence in situ hybridization (FISH) is a molecular genetic test used to identify chromosomal abnormalities and other genetic changes in the leukemia cells, or blasts. It uses special DNA probes labelled with fluorescent dyes. FISH is used to tell apart leukemias that look the same but that have different genetic abnormalities and may need to be treated differently.
Polymerase chain reaction (PCR) is a method used to make many copies of a particular gene segment so that it can be tested in the lab. PCR is used to find DNA mutations, inversions or deletions that are linked with certain types of leukemia. It is useful in diagnosing and determining the prognosis for a specific type of leukemia.
Bone marrow aspiration and biopsy
During a bone marrow aspiration and biopsy, cells are removed from the bone marrow so they can be tested in a lab. The report from the lab will confirm whether or not there are leukemia cells in the sample and, if so, the type of leukemia.
Lumbar puncture
A lumbar puncture, or spinal tap, removes a small amount of cerebrospinal fluid (CSF) from the space around the spine to look at it under a microscope. CSF is the fluid that surrounds the brain and spinal cord.
A lumbar puncture is done to see if cancer has spread to the spinal fluid.
Lymph node biopsy
A lymph node biopsy is a type of surgical biopsy. It is called an excisional biopsy because the lymph node is completely removed. Sometimes the lymph node cannot be completely removed; instead a portion of the lymph node is removed as a core biopsy. Doctors (pathologists) then look at the lymph node under a microscope to find out if there are cancer cells in it, identify the type of cancer and find out how quickly the cancer cells are growing.
Chest x-ray
An x-ray uses small doses of radiation to make an image of the body’s structures on film. It is used to look for:
- enlarged lymph nodes in the centre of the chest (called mediastinal lymph nodes)
- enlarged thymus gland
- buildup of fluid between the lungs and the walls of the chest (called pleural effusion)
- lung infection (called pneumonia)
CT scan
A computed tomography (CT) scan uses special x-ray equipment to make 3-D and cross-sectional images of organs, tissues, bones and blood vessels inside the body. A computer turns the images into detailed pictures.
A CT scan may be used to look at the spleen and liver to see if they are larger than normal, or enlarged. It can also be used to check if lymph nodes around the heart, near the trachea (windpipe) or in the back of the abdomen are enlarged.
MRI
Magnetic resonance imaging (MRI) uses powerful magnetic forces and radiofrequency waves to make cross-sectional images of organs, tissues, bones and blood vessels. A computer turns the images into 3-D pictures.
MRI is most often used when doctors think that the leukemia has spread to the brain.
Ultrasound
Ultrasound uses high-frequency sound waves to make images of structures in the body. It is used to see if internal organs, such as the kidneys, liver or spleen, have been affected by leukemia.
Treatments for leukemia
If you have leukemia, your healthcare team will make a treatment plan just for you. It will be based on your needs and may involve a combination of different treatments. When your healthcare team decides which treatments to offer you for leukemia, they take the following into consideration:
- the type of leukemia
- your age
- the presence of chromosomal (genetic) abnormalities
- your overall health
If leukemia is present, the following treatment options may be used.
- Chemotherapy is the main treatment for many types of leukemia. Find out more about chemotherapy.
- Stem cell transplantation may be an option for some people under the age of 55.
- Radiation therapy is most often given to prevent the spread of leukemia to the central nervous system (CNS) or to treat leukemia that has spread to the CNS. It is also used to prepare the bone marrow for a stem cell transplant.
- Targeted therapy is offered for certain types of leukemia.
- Watchfulness is a treatment option for some people with chronic lymphocytic leukemia (CLL).
- Supportive treatment helps control the expected complications of leukemia and its treatments.
Treatment by type
The healthcare team will develop a treatment plan based on your needs and the type of leukemia you have. Find out more about the treatments for the 4 main types of leukemia:
- acute lymphoblastic leukemia (ALL)
- acute myelogenous leukemia (AML)
- chronic lymphocytic leukemia (CLL)
- chronic myelogenous leukemia (CML)
Other types of treatment may be offered for other types of leukemia.
Monitoring
Follow-up after treatment is an important part of caring for people with cancer. You will need to have regular follow-up visits. These visits allow the healthcare team to monitor your progress and to know how you are recovering from treatment.
Survival statistics for acute myelogenous leukemia
Acute myelogenous leukemia (AML) survival statistics are very general estimates and should be interpreted with caution. Since they are based on the experience of groups of people, they cannot predict the chances of survival of any particular person.
There are many different methods to assess and record cancer survival statistics. Your doctor can explain the statistics for AML and what they mean to you.
Net survival
Net survival represents the probability of surviving cancer in the absence of other causes of death. It is used to estimate the percentage of people who will survive their cancer.
Overall survival for AML
People with AML should be treated. Without treatment, they can only survive for days or even weeks.
With current treatment regimens, 65-70% of people with AML achieve complete remission, which means leukemia cells are not seen in their bone marrow after induction therapy. Adults over the age of 60 usually have a lower response rate. About 25 to 40% of people over the age of 60 survive 3 years or more.
If you do an allogeneic stem cell transplant during the first remission, the 5-year recurrence-free survival rate is 30 to 50%. If there has been no recurrence in the 2 years after the stem cell transplant, the person has an 80% chance of remaining in complete remission for a long time.
People who have received intensive consolidation therapy and those who have received an allogeneic stem cell transplant have similar survival rates. They are slightly lower for people who receive an autologous stem cell transplant.
Survival for acute promyelocytic leukemia
The treatments offered and survival statistics for acute promyelocytic leukemia (APL) differ from those for other types of AML. After achieving complete remission, 70 to 90% of people with APL survive a long time, and doctors consider them to be cured.
Survival questions
If you have AML, talk to your doctor about your prognosis. The prognosis is based on many factors including the following:
- medical background
- type of cancer
- Stadium
- characteristics of cancer
- selected treatments
- response to treatment
Only a doctor who is familiar with these factors will be able to look at all of this data together with the survival statistics to arrive at a prognosis.
Life expectancy
In children, leukemia often has a good prognosis: more than 80% of children with acute lymphoblastic leukemia recover definitively, and less than 20% relapse.
In adults, the results are less satisfactory: a very small number of leukemias has a good prognosis. The treatments are heavier, have side effects, and relapses are more frequent than in children. “While there is still a lot of progress to be made to improve the management of leukemia, recent or developing strategies offer immense hope. In recent years, new therapeutic strategies have made it possible to improve the historically insufficient results. . These consist in using therapeutic antibodies capable of specifically targeting leukemia cells in order to bring them closer to our cells of the immune system, and to destroy them (so-called bispecific antibody technique). arm “our immune system so that it destroys diseased cells more effectively (a technique known as CAR-t cells). Finally, small molecules have been developed so that they can specifically inhibit proteins responsible for leukemia (so-called therapies targeted) “, specifies Professor Coppo. “The death of patients is most often due to the fact that they become unable to fight off infections which can be overwhelming.” Death can also be linked to severe bleeding.
List of all Cancers
The word “cancer” is a generic term for a large group of diseases that can affect any part of the body. We also speak of malignant tumors or neoplasms. One of the hallmarks of cancer is the rapid multiplication of abnormal growing cells, which can invade nearby parts of the body and then migrate to other organs. This is called metastasis, which is the main cause of death from cancer. Types of cancer (in alphabetical order of the area concerned):
Sources: PinterPandai, Seattle Cancer Care Alliance, Everyday Health, American Society of Hematology, Harvard Medical School, U.S. Department of Health and Human Services, Mayo Clinic, Leukaemia Care UK
Photo credit: Wikimedia Commons
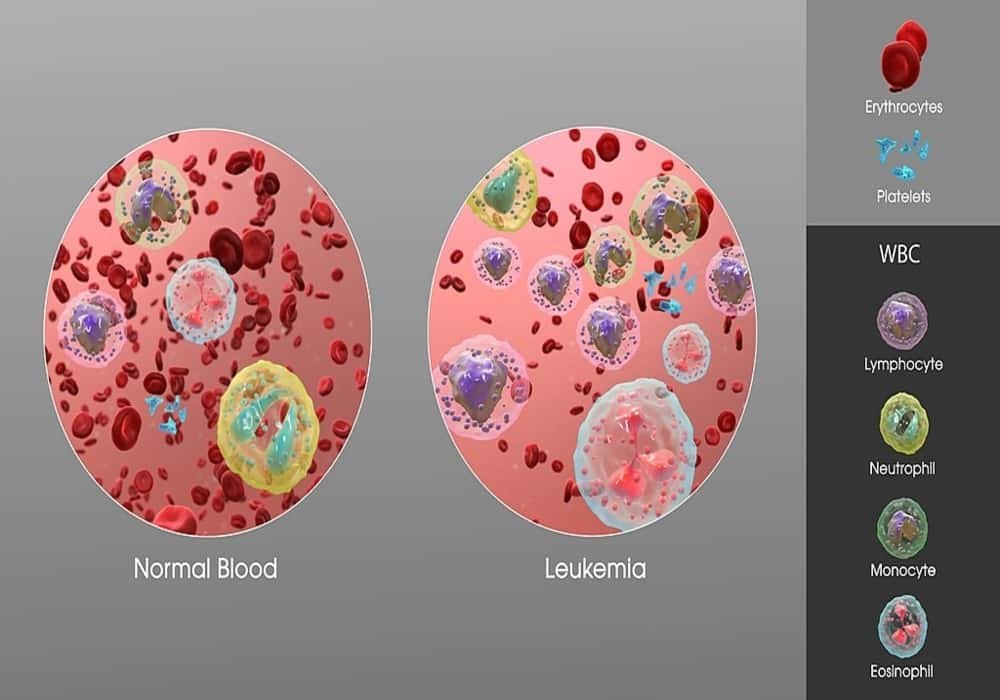
Photo explaination: showing an increase in white blood cells of a person suffering from Leukemia.